🐍 Snake Bite – Comprehensive Clinical Guide
1. Definition
A snake bite is an injury caused by the bite of a snake, which may result in envenomation (toxic venom injection) or may be non-venomous (dry bite). Snake envenomation is a medical emergency due to rapid systemic effects.
2. Epidemiology (India-focused)
- High incidence in rural areas, farmers, laborers
- Peak during monsoon and night
- WHO-recognized Neglected Tropical Disease
- Major venomous snakes in India: “Big Four”
* Cobra
* Krait
* Russell’s viper
* Saw-scaled viper
3. Types of Snake Bite
A. Non-venomous bite
- No venom injection
- Local pain, anxiety only
B. Venomous bite
- Neurotoxic – Cobra, Krait
- Hemotoxic / Vasculotoxic – Vipers
- Myotoxic – Sea snakes
- Mixed toxicity – Some cobras, vipers
4. Venom Pathophysiology
| Venom Type | Mechanism |
| ----------- | --------------------------------------------------------- |
| Neurotoxic | Blocks neuromuscular transmission (pre- or post-synaptic) |
| Hemotoxic | Activates clotting → consumption coagulopathy |
| Cytotoxic | Local tissue necrosis |
| Myotoxic | Muscle breakdown → rhabdomyolysis |
| Cardiotoxic | Arrhythmias, myocardial depression |
5. Clinical Features
A. Local Manifestations
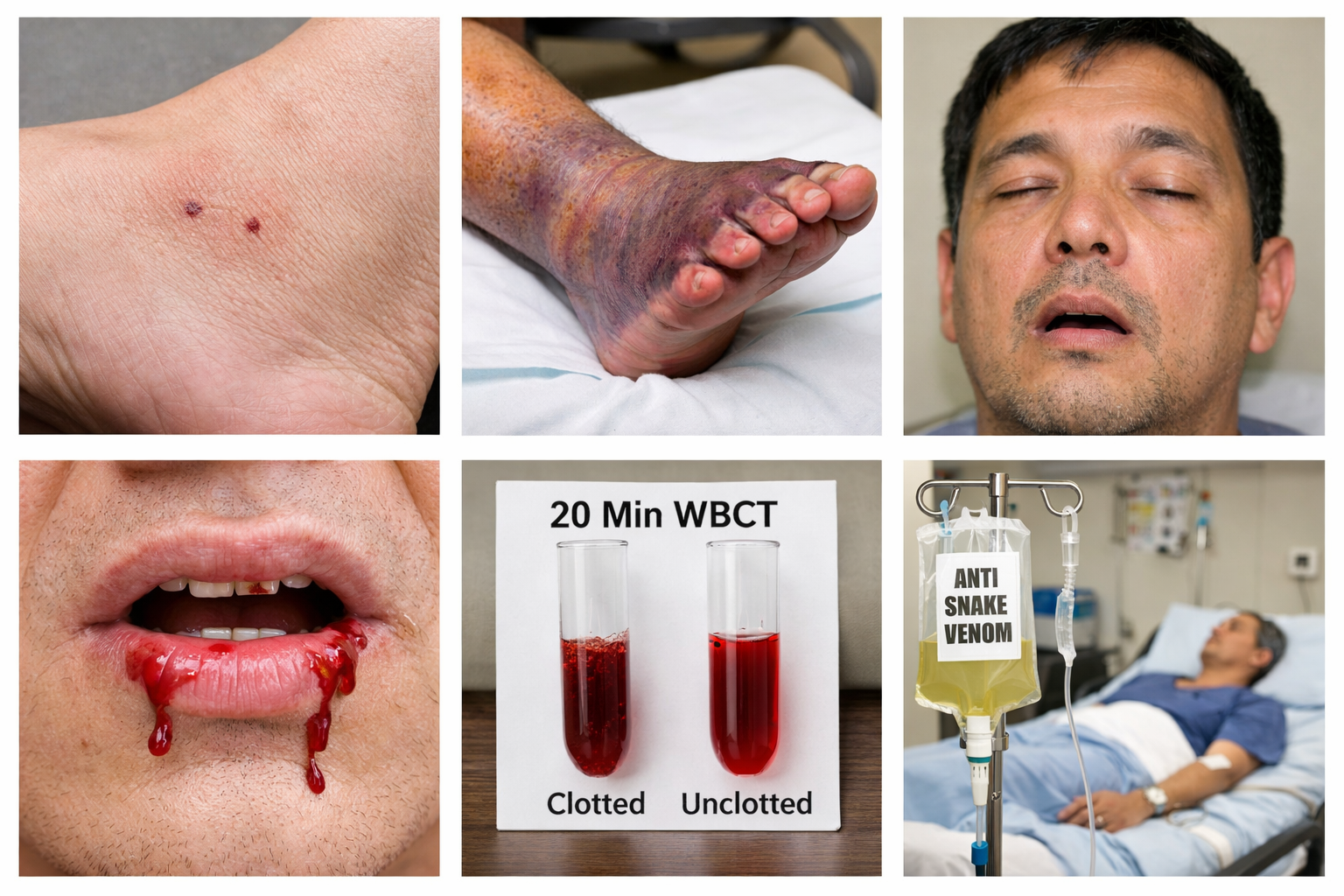
- Fang marks
- Pain, swelling
- Bleeding
- Blisters, necrosis
- Compartment syndrome
B. Systemic Manifestations
1. Neurotoxic Envenomation
- Ptosis (earliest sign)
- Ophthalmoplegia
- Dysarthria
- Dysphagia
- Respiratory muscle paralysis
- Coma
2. Hemotoxic Envenomation
- Spontaneous bleeding (gums, urine, GI)
- Hematemesis, melena
- DIC
- Hypotension, shock
- Acute kidney injury (AKI)
3. Myotoxic Envenomation
- Muscle pain
- Dark urine (myoglobinuria)
- Elevated CK
- Renal failure
6. Dry Bite Indicators
- No local swelling
- No progression after 24 hours
- Normal coagulation
- No neuro signs
7. First Aid – DOs and DON’Ts
✅ DO
- Reassure patient
- Immobilize limb
- Remove tight clothing/jewelry
- Transport urgently to hospital
❌ DON’T
- No tourniquet
- No incision/suction
- No electric shock
- No traditional remedies
- No ice or chemicals
8. Hospital Evaluation
A. History
- Time of bite
- Snake identification (if safe)
- First aid done
B. Examination
- Vitals
- Local swelling progression
- Neuro exam
- Bleeding sites
- Urine output
9. Investigations
Bedside
- 20-minute whole blood clotting test (20WBCT)
Laboratory
- CBC
- PT/INR, aPTT
- Serum creatinine, urea
- LFT
- Serum CK
- Urinalysis (hematuria, myoglobin)
10. Indications for Anti-Snake Venom (ASV)
- Neuroparalysis
- Spontaneous bleeding
- Incoagulable blood (20WBCT)
- Rapidly progressive swelling
- AKI or shock
11. Anti-Snake Venom (ASV)
Indication
Confirmed or suspected venomous bite with systemic signs
Mechanism of Action
- Neutralizes circulating venom
Dosing (India – Polyvalent ASV)
- Initial: 8–10 vials IV
- Severe cases: up to 20 vials
- Repeat dose based on clinical response
Route
- IV infusion over 1 hour
Pharmacokinetics (Summary)
- Acts only on free venom
- No effect on venom already bound to tissues
Adverse Effects
- Anaphylaxis
- Fever, chills
- Serum sickness (5–10 days later)
Contraindications
- None in life-threatening envenomation
Drug Interactions
- None clinically significant
Monitoring
- Vitals
- Signs of allergy
- Coagulation profile
- Neurological status
Patient Counselling
- ASV saves life
- Allergic reactions are manageable
- Delayed reactions possible
12. Management of ASV Reactions
Mild
- Antihistamines
Severe (Anaphylaxis)
- Adrenaline IM
- IV fluids
- Oxygen
- Corticosteroids
13. Supportive Management
Neurotoxic Bite
- Early intubation and ventilation
- Neostigmine + atropine trial (post-synaptic block)
Hemotoxic Bite
- Fresh frozen plasma
- Platelets if bleeding
- Dialysis for AKI
Local Complications
- Elevation of limb
- Fasciotomy (only if confirmed compartment syndrome)
- Wound care
14. Special Situations
Pregnancy
- ASV is safe and lifesaving
Children
- Same ASV dose as adults
Dry Bite
- Observation for 24 hours
- No ASV required
15. Prognosis
- Good if treated early
- Poor outcomes with:
* Delayed treatment
* Respiratory failure
* Renal failure
* Massive bleeding
16. Prevention
- Protective footwear
- Use torch at night
- Avoid sleeping on floor
- Educate rural population
17. Key Exam Pearls
- 20WBCT is bedside diagnostic test
- ASV dose is same in adults and children
- ASV neutralizes venom, not tissue damage
- Respiratory failure is leading cause of death in neurotoxic bites