Definition
Edema is the abnormal accumulation of fluid in the interstitial (extravascular) spaces, leading to visible or palpable swelling of tissues. It may be localized or generalized, pitting or non-pitting, and acute or chronic.
Pathophysiology (core mechanisms)
Edema results from imbalance between forces governing capillary fluid exchange (Starling forces) and lymphatic drainage:
- ↑ Capillary hydrostatic pressure
→ pushes fluid out of capillaries
Examples: heart failure, venous obstruction, fluid overload
- ↓ Plasma oncotic (colloid osmotic) pressure
→ reduced reabsorption due to low albumin
Examples: nephrotic syndrome, liver cirrhosis, malnutrition
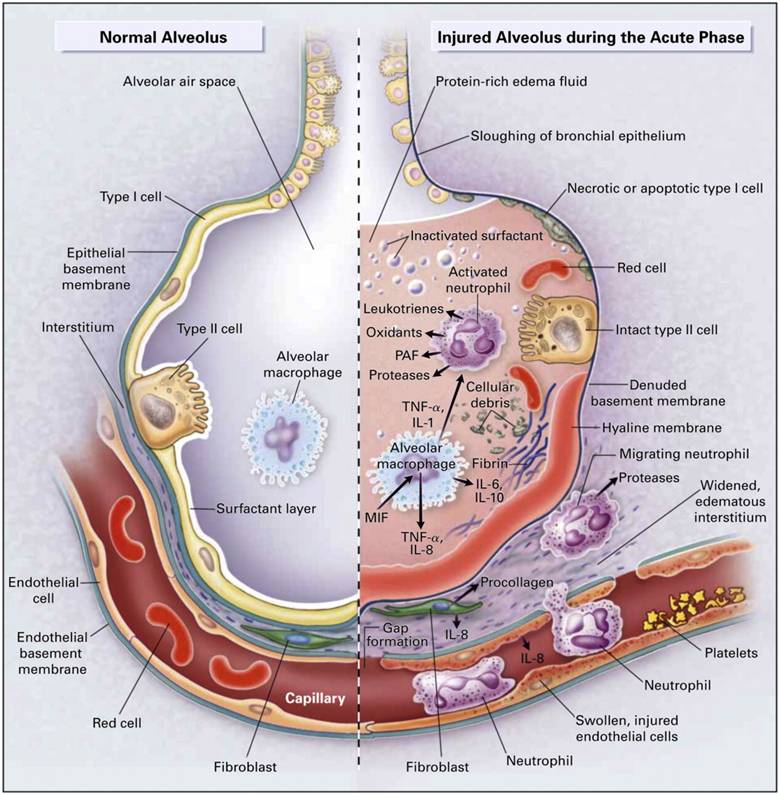
- ↑ Capillary permeability
→ protein-rich fluid leaks into interstitium
Examples: inflammation, burns, sepsis, allergic reactions
- Lymphatic obstruction or failure
→ impaired removal of interstitial fluid
Examples: filariasis, malignancy, post-surgery/radiation
- Renal sodium and water retention
→ expands plasma volume, worsening edema
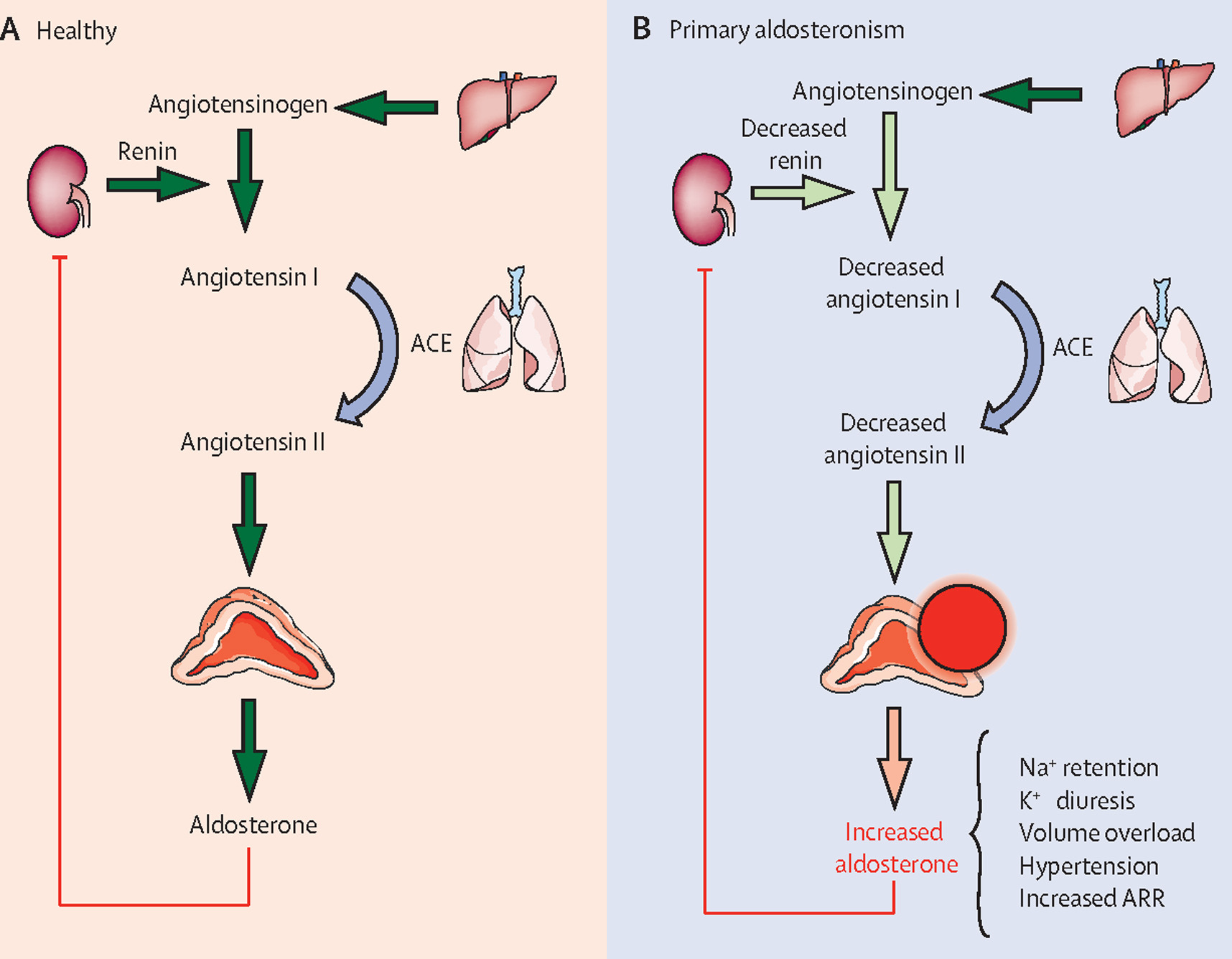
Examples: chronic kidney disease, heart failure, hyperaldosteronism
Classification
By distribution
- Localized edema: one limb/organ (DVT, cellulitis)
- Generalized edema (anasarca): whole body (nephrotic syndrome, CHF)
By nature
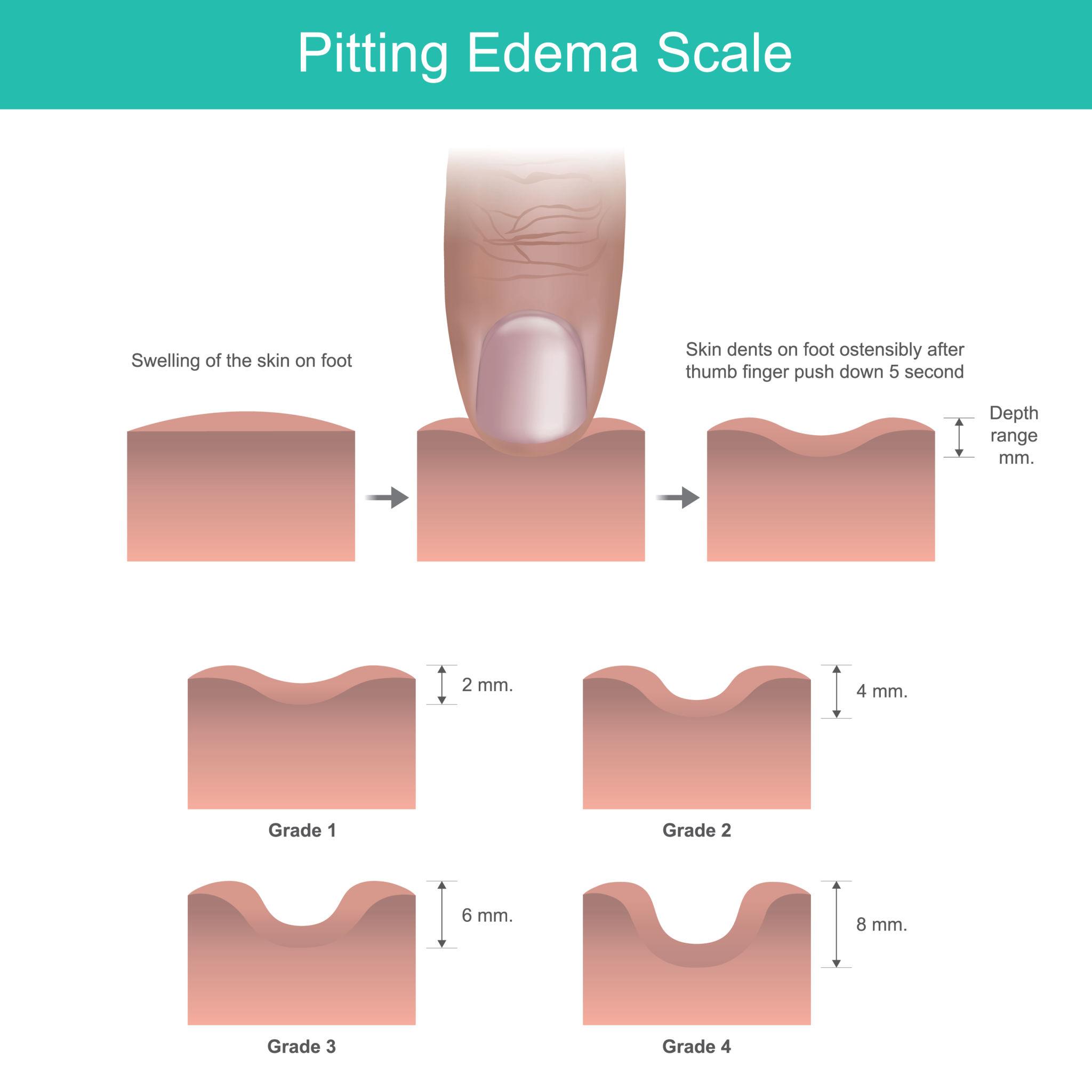
- Pitting edema: indentation persists after pressure
(cardiac, renal, hepatic causes)
- Non-pitting edema: no indentation
(lymphedema, myxedema)
By timing
- Dependent edema: worse in evenings (cardiac)
- Periorbital edema: worse in mornings (renal)
Causes / Etiology
Cardiac
- Congestive heart failure (right-sided > systemic edema)
Renal
- Nephrotic syndrome
- Acute/chronic kidney disease
Hepatic
- Cirrhosis (hypoalbuminemia + portal hypertension)
Endocrine
- Hypothyroidism (myxedema)
- Hyperaldosteronism
Vascular
- Deep vein thrombosis
- Chronic venous insufficiency
Lymphatic
- Filariasis
- Malignancy
- Post-surgical or post-radiation damage
Inflammatory / Allergic
- Angioedema
- Cellulitis
Drug-induced
- Calcium channel blockers (e.g., amlodipine)
- NSAIDs
- Corticosteroids
- Thiazolidinediones
Clinical features
General
- Swelling of affected area
- Weight gain
- Tightness or heaviness
Specific patterns
- Periorbital edema: renal disease
- Bilateral pedal edema: cardiac, hepatic, renal
- Unilateral limb edema: DVT, lymphatic obstruction
- Non-pitting, firm edema: lymphedema, myxedema
- Associated symptoms:
* Dyspnea (heart failure)
* Ascites, jaundice (liver disease)
* Frothy urine (nephrotic syndrome)
Examination
- Pitting test: press thumb for 10–15 seconds
- Grade of pitting:
* 1+: mild (2 mm)
* 2+: moderate (4 mm)
* 3+: deep (6 mm)
* 4+: very deep (8 mm)
- Check JVP, lung crepitations, hepatosplenomegaly, skin changes
Investigations
Basic
- CBC
- Serum electrolytes
- Blood urea, serum creatinine
- Liver function tests
- Serum albumin
- Urine routine and protein quantification
Targeted
- ECG, echocardiography: cardiac cause
- Ultrasound abdomen: liver, kidneys, ascites
- Doppler ultrasound: DVT / venous insufficiency
- TSH: suspected hypothyroidism
- 24-hour urine protein: nephrotic syndrome
Differential diagnosis
- Lipedema
- Obesity-related swelling
- Cellulitis
- Hematoma
- Myxedema
- Compartment syndrome (acute painful swelling)
Management (stepwise)
1. Treat underlying cause
- Heart failure → optimize cardiac therapy
- Renal disease → proteinuria control, renal-specific care
- Liver disease → manage cirrhosis and portal hypertension
- DVT → anticoagulation
- Hypothyroidism → thyroid hormone replacement
2. Non-pharmacologic measures
- Salt restriction (usually <2 g/day)
- Fluid restriction (if indicated)
- Leg elevation
- Compression stockings (venous edema)
- Weight monitoring
- Skin care to prevent breakdown/infection
3. Pharmacologic treatment
Loop diuretics (e.g., furosemide)
- Indication: moderate–severe edema, heart failure, renal edema
- Mechanism: inhibits Na-K-2Cl cotransporter in thick ascending loop
- Dose:
* Adult: 20–80 mg/day PO/IV (titrate)
* Pediatric: 1–2 mg/kg/dose
- Adverse effects: hypokalemia, dehydration, hypotension, ototoxicity
- Contraindications: severe hypovolemia, anuria
- Monitoring: electrolytes, renal function, BP
- Counseling: morning dosing, potassium-rich diet if advised
Thiazide diuretics
- Use: mild edema, adjunct to loop diuretics
- Risks: hyponatremia, hypokalemia, hyperuricemia
Potassium-sparing diuretics (e.g., spironolactone)
- Indication: cirrhosis, heart failure, hyperaldosteronism
- Mechanism: aldosterone antagonist
- Dose: 25–100 mg/day
- Adverse effects: hyperkalemia, gynecomastia
- Monitoring: serum potassium
Albumin infusion
- Use: severe hypoalbuminemia with edema (e.g., nephrotic syndrome)
- Often combined with loop diuretics
Antihistamines / steroids
- Use: allergic or inflammatory edema
Complications
- Skin breakdown and ulcers
- Secondary infection (cellulitis)
- Reduced mobility
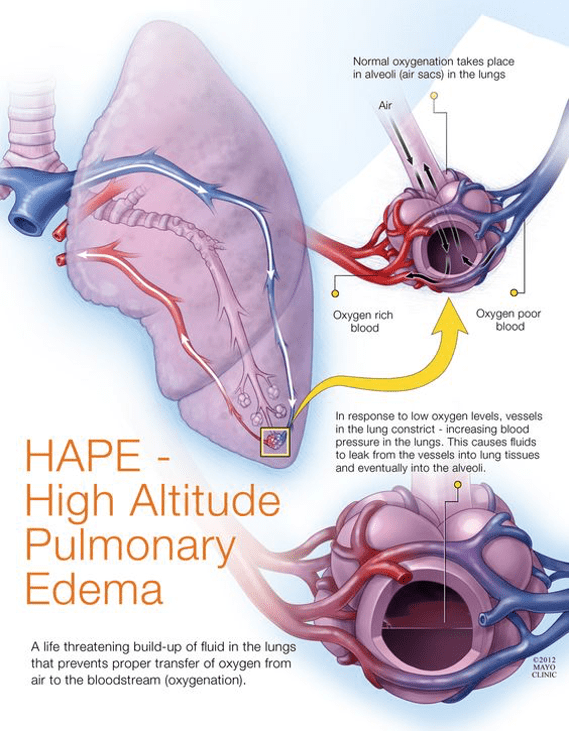
- Pulmonary edema (life-threatening)
- Delayed wound healing