1. Overview of CVS Physiology
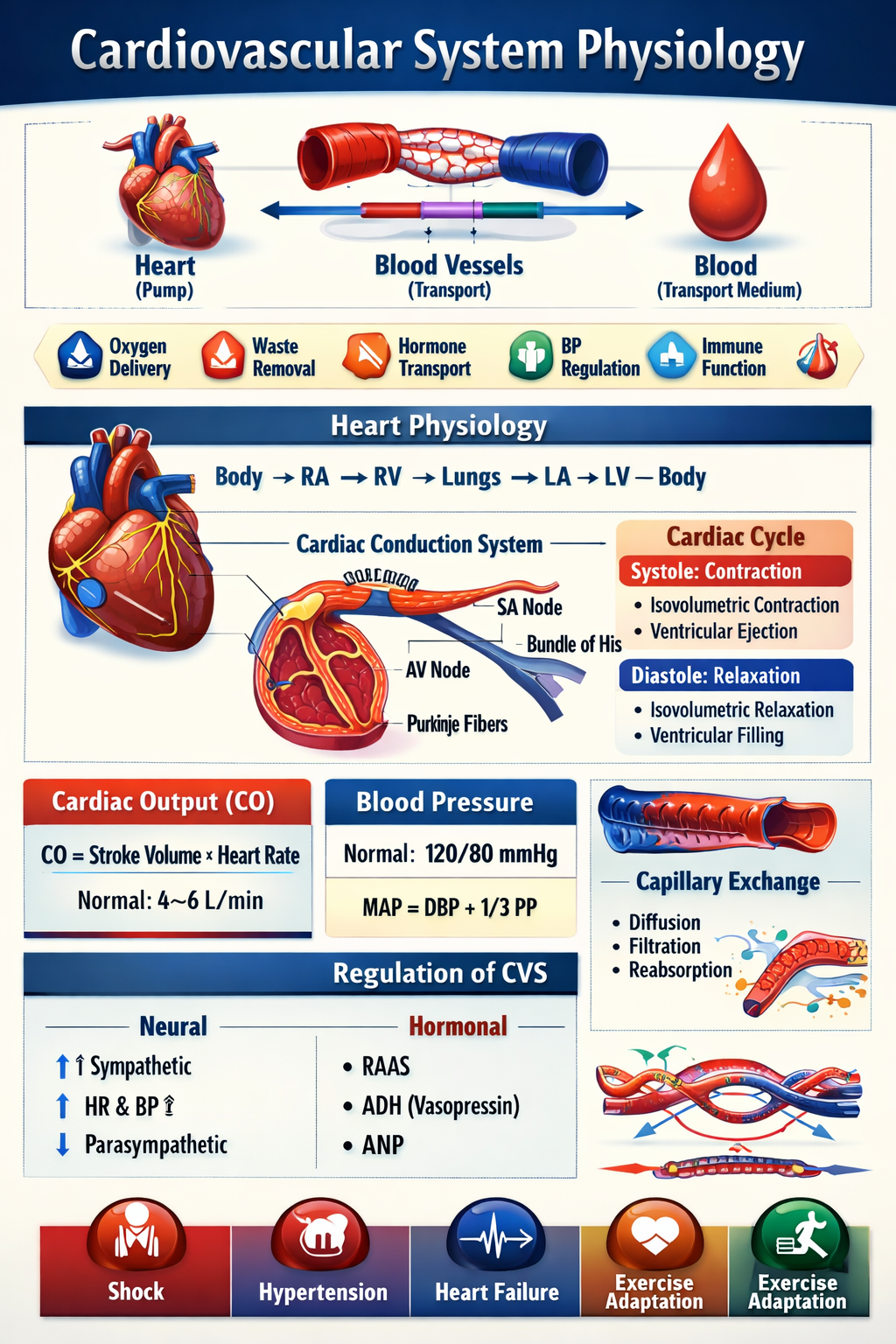
The cardiovascular system ensures continuous circulation of blood to deliver oxygen, nutrients, hormones, and remove metabolic waste. It maintains blood pressure, tissue perfusion, acid–base balance, and body temperature.
Main Components
- Heart → Pump
- Blood vessels → Transport channels
- Blood → Transport medium
2. Functions of the Cardiovascular System
- Oxygen and nutrient delivery
- Removal of carbon dioxide and waste
- Immune defense
- Temperature regulation
- Hormone transport
- Maintenance of blood pressure
- Regulation of fluid balance
- Homeostasis and metabolic support
3. Heart Physiology
3.1 Structure and Function
The heart has four chambers:
- Right atrium
- Right ventricle
- Left atrium
- Left ventricle
Blood Flow Pathway
Body → Right atrium → Right ventricle → Lungs → Left atrium → Left ventricle → Body
3.2 Cardiac Muscle Physiology
Unique Features
- Striated and involuntary
- Intercalated discs (gap junctions)
- Automatic rhythmicity
Key Properties
- Automaticity → Self-excitation
- Conductivity → Impulse transmission
- Excitability → Response to stimulus
- Contractility → Force of contraction
- Refractory period → Prevents tetany
4. Electrical Activity of the Heart
4.1 Cardiac Conduction System
- Sinoatrial (SA) node → Pacemaker
- Atrioventricular (AV) node
- Bundle of His
- Purkinje fibers
Heart Rate
- Normal adult: 60–100 bpm
4.2 Action Potentials
Pacemaker Cells
Phases: Slow depolarization → Threshold → Repolarization
Ventricular Muscle Cells
Phases:
- Phase 0: Rapid depolarization (Na⁺ influx)
- Phase 1: Initial repolarization
- Phase 2: Plateau (Ca²⁺ influx)
- Phase 3: Repolarization (K⁺ efflux)
- Phase 4: Resting potential
Significance
- Plateau prevents sustained contraction
- Coordinates effective pumping
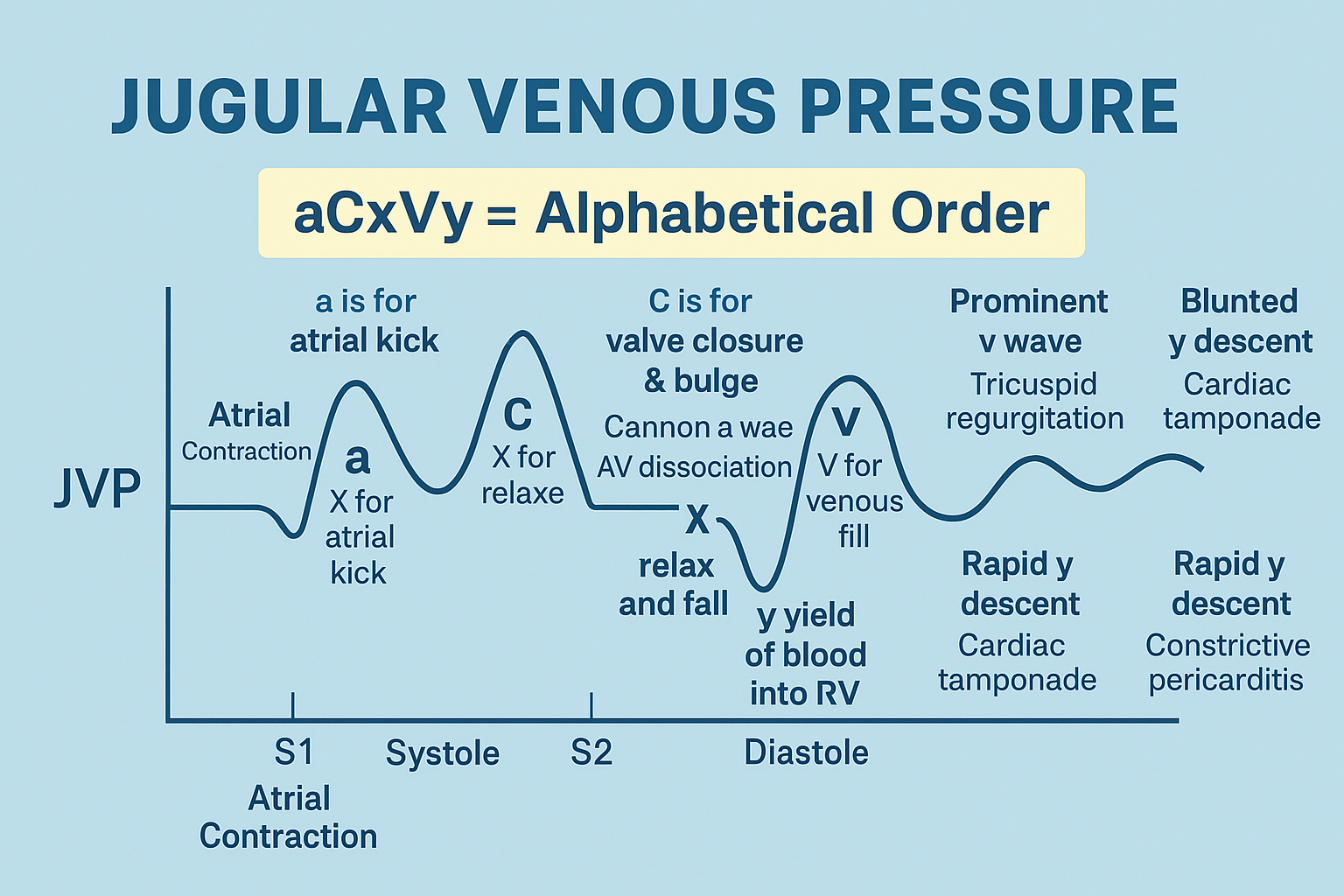
5. Cardiac Cycle Physiology
Phases
Systole
- Isovolumetric contraction
- Ventricular ejection
Diastole
- Isovolumetric relaxation
- Rapid filling
- Atrial contraction
Heart Sounds
- S1 → AV valve closure
- S2 → Semilunar valve closure
6. Cardiac Output (CO)
Formula
CO = Stroke Volume × Heart Rate
Normal Value
4–6 L/min (rest)
6.1 Stroke Volume Determinants
Preload
Ventricular filling volume
(Frank–Starling law)
Afterload
Resistance against ventricular ejection
Contractility
Strength of myocardial contraction
Increased by sympathetic stimulation
7. Blood Pressure Physiology
Normal BP
120/80 mmHg
Determinants
- Cardiac output
- Peripheral vascular resistance
- Blood volume
- Arterial elasticity
7.1 Mean Arterial Pressure (MAP)
MAP = Diastolic BP + 1/3 Pulse Pressure
8. Hemodynamics (Blood Flow Dynamics)
Laminar Flow
Smooth, parallel blood movement
Poiseuille’s Law
Flow ∝ Radius⁴
(Small radius change → major flow change)
Vascular Resistance
Highest in arterioles
Primary regulators of blood pressure
9. Blood Vessel Physiology
Arteries
- High pressure
- Elastic walls
Arterioles
- Resistance vessels
- BP control
Capillaries
- Exchange vessels
Veins
- Blood reservoir
- Venous return system
10. Microcirculation and Capillary Exchange
Exchange Mechanisms
- Diffusion
- Filtration
- Reabsorption
Starling Forces
- Capillary hydrostatic pressure
- Plasma oncotic pressure
11. Venous Return Physiology
Mechanisms
- Skeletal muscle pump
- Respiratory pump
- Venous valves
- Sympathetic venoconstriction
12. Coronary Circulation Physiology
- Supplies myocardium
- Occurs mainly during diastole
- Regulated by metabolic demand
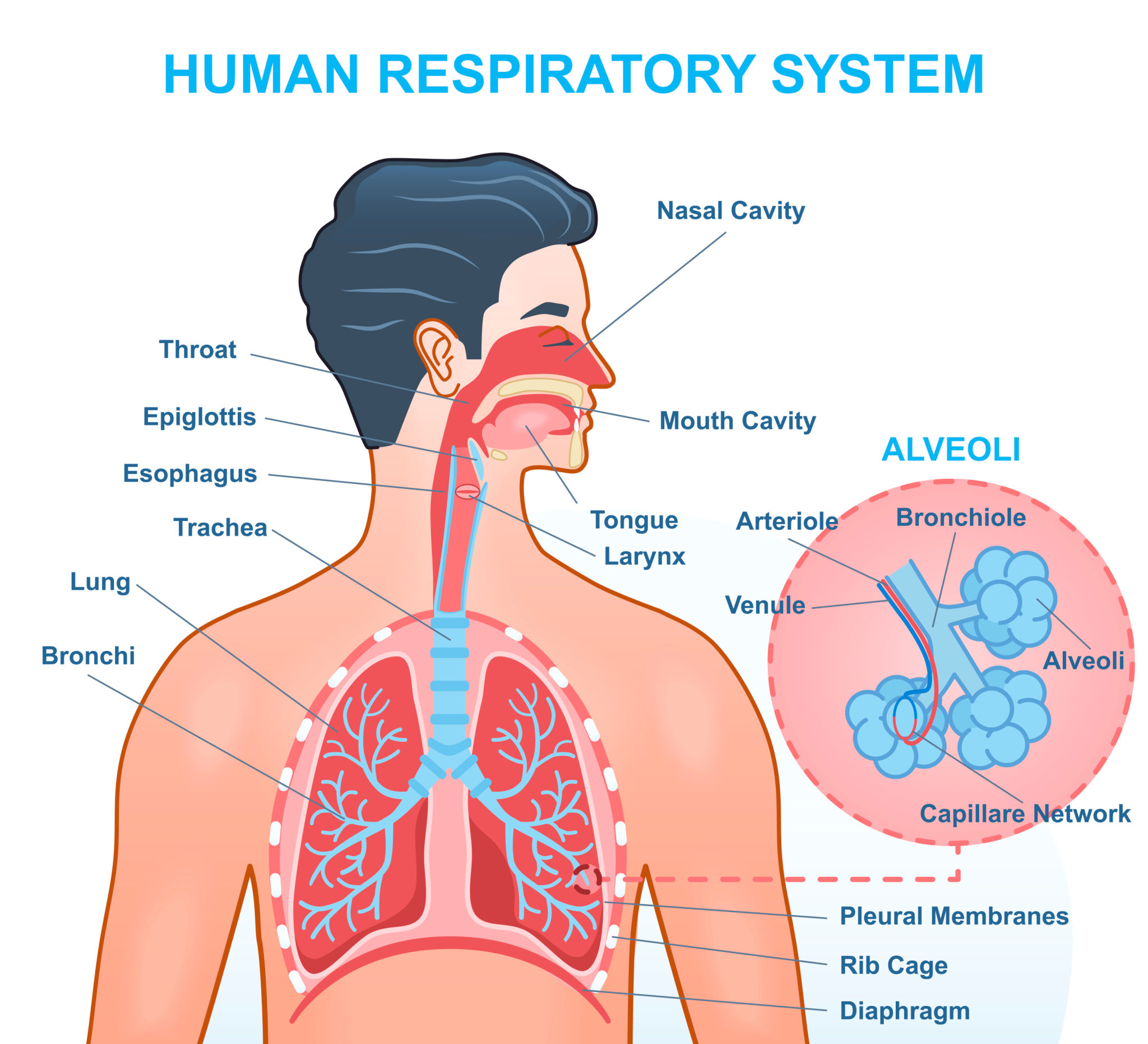
13. Pulmonary Circulation Physiology
- Low-pressure system
- Gas exchange function
- Regulates blood oxygenation
14. Regulation of Cardiovascular Function
14.1 Neural Regulation
Sympathetic
- ↑ Heart rate
- ↑ Contractility
- Vasoconstriction
Parasympathetic (Vagus)
- ↓ Heart rate
14.2 Reflex Regulation
Baroreceptor Reflex
Responds to BP changes
Chemoreceptor Reflex
Responds to O₂, CO₂, pH
14.3 Hormonal Regulation
- Renin–Angiotensin–Aldosterone System (RAAS)
- ADH (Vasopressin)
- Atrial Natriuretic Peptide (ANP)
- Adrenaline/Noradrenaline
15. Exercise and CVS Adaptation
During Exercise
- ↑ Cardiac output
- ↑ Heart rate
- ↑ Stroke volume
- Redistribution of blood to muscles
Long-Term Training Effects
- Increased cardiac efficiency
- Lower resting heart rate
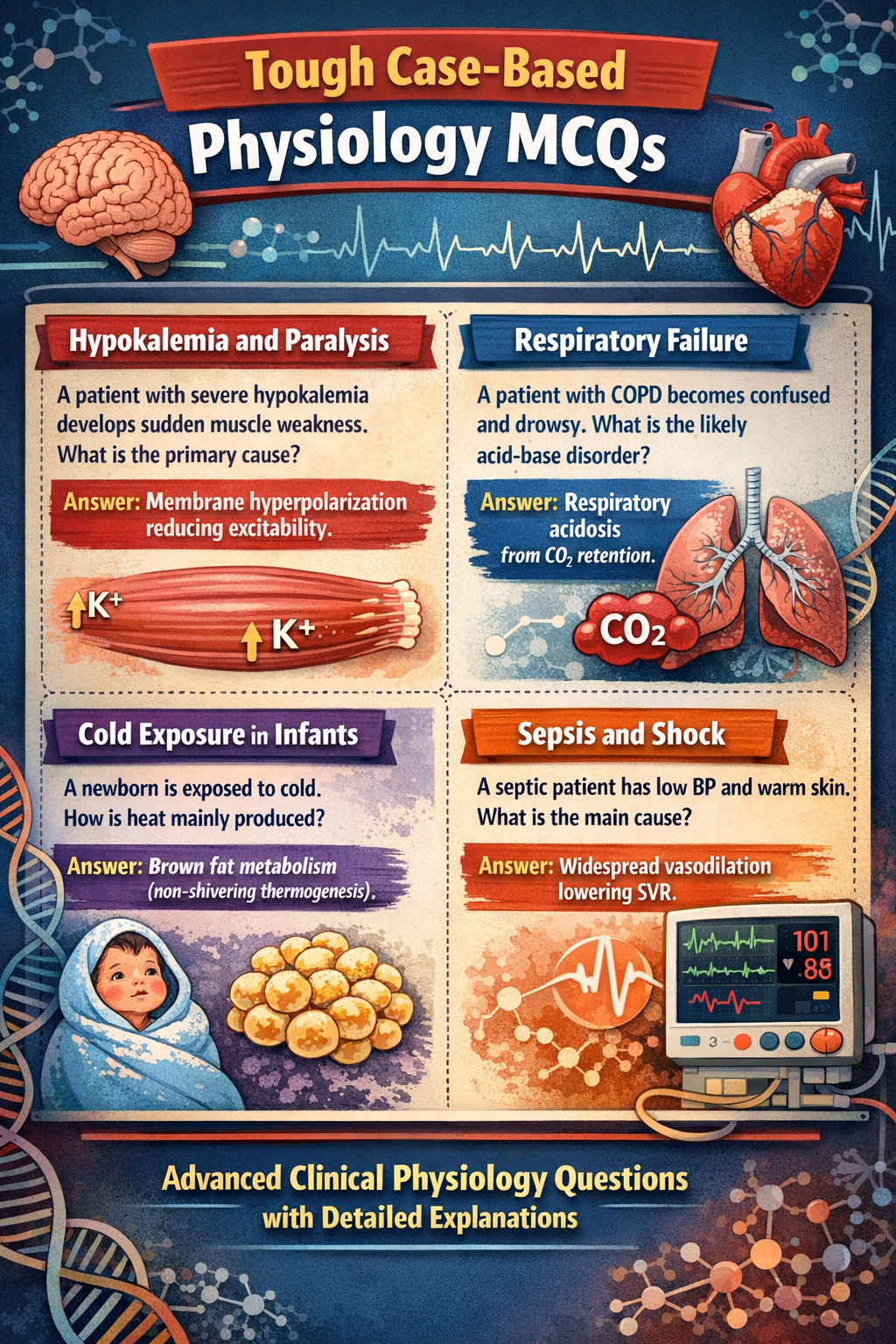
16. Shock and CVS Physiology
Types
- Hypovolemic
- Cardiogenic
- Septic
- Neurogenic
Key Feature
Reduced tissue perfusion
17. Aging and Cardiovascular Changes
- Reduced arterial elasticity
- Increased BP
- Decreased cardiac reserve
18. Clinical Relevance Summary
| Parameter | Normal Value |
| ----------------- | ------------ |
| Heart Rate | 60–100 bpm |
| Cardiac Output | 4–6 L/min |
| Stroke Volume | 70 mL |
| Blood Pressure | 120/80 mmHg |
| Ejection Fraction | 55–70% |