BLOOD TRANSFUSION AND MASSIVE BLOOD TRANSFUSION PROTOCOL
(Comprehensive Clinical Guide)
1. BLOOD TRANSFUSION
1.1 Definition
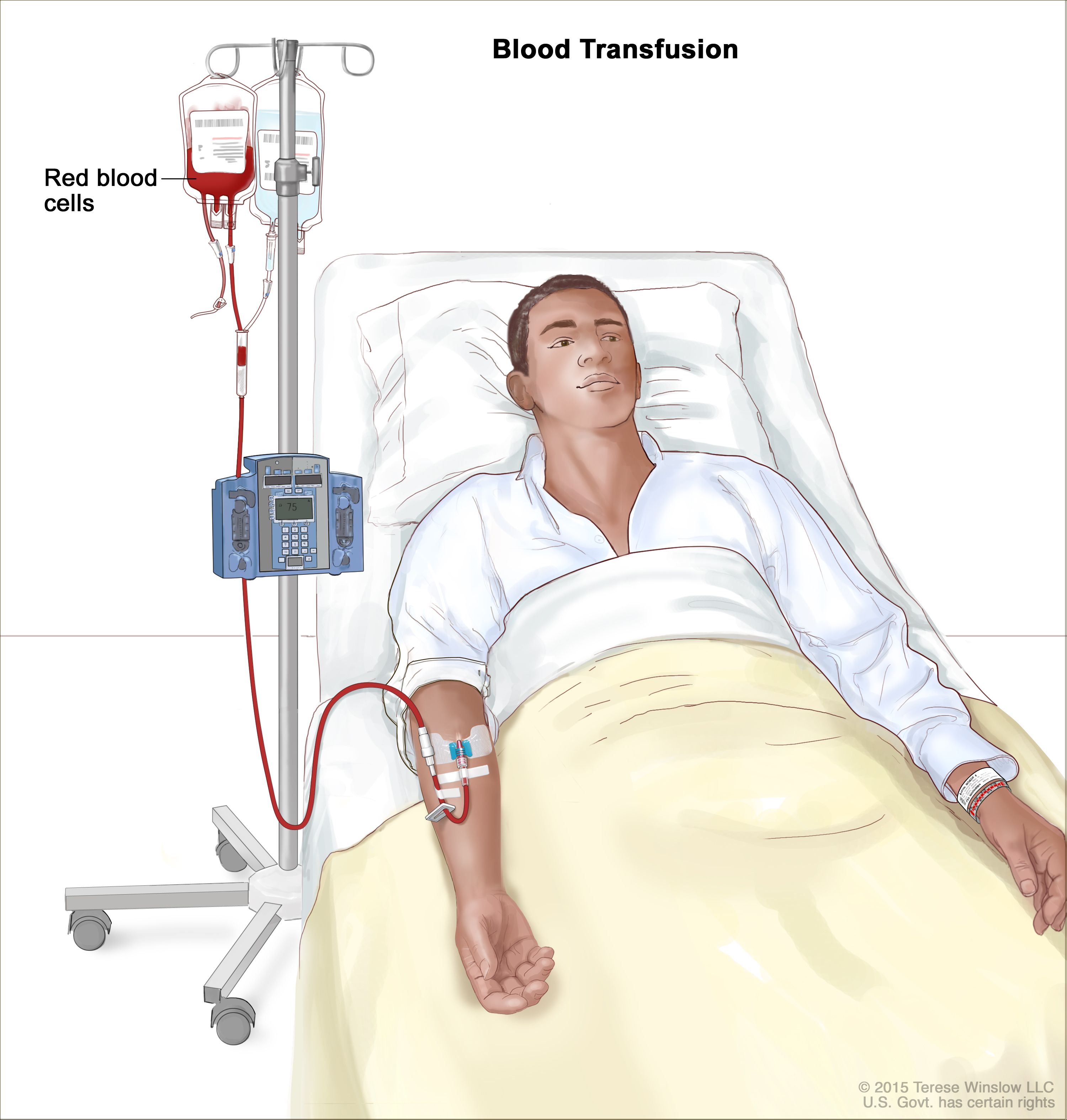
Blood transfusion is the intravenous administration of whole blood or specific blood components to restore circulating volume, improve oxygen-carrying capacity, or correct coagulation abnormalities.
1.2 Types of Blood Products
A. Whole Blood
- Contains RBCs, plasma, platelets
- Rarely used (trauma with massive hemorrhage in select centers)
B. Packed Red Blood Cells (PRBCs)
- Raises oxygen delivery
- 1 unit ↑ Hb by ~1 g/dL (adult)
C. Platelet Concentrates
- Random donor platelets (RDP)
- Single donor platelets (SDP/apheresis)
D. Fresh Frozen Plasma (FFP)
- All coagulation factors
- Volume ~200–250 mL/unit
E. Cryoprecipitate
- Rich in fibrinogen, Factor VIII, XIII, vWF
F. Plasma Derivatives
- Albumin, immunoglobulins, factor concentrates
1.3 Indications for Blood Transfusion
A. PRBC Transfusion
| Clinical Situation | Transfusion Threshold |
| -------------------------- | --------------------- |
| Stable, non-bleeding adult | Hb <7 g/dL |
| Cardiovascular disease | Hb <8 g/dL |
| Ongoing bleeding/shock | Clinical judgment |
| Perioperative | Hb <7–8 g/dL |
B. Platelet Transfusion
| Situation | Platelet Count |
| ----------------------- | -------------- |
| Prophylaxis | <10,000/µL |
| Fever/sepsis | <20,000/µL |
| Active bleeding/surgery | <50,000/µL |
| Neurosurgery | <100,000/µL |
C. FFP
- Active bleeding with INR >1.5
- DIC
- Liver disease with bleeding
- Massive transfusion
D. Cryoprecipitate
- Fibrinogen <150–200 mg/dL
- DIC, massive hemorrhage
- Congenital hypofibrinogenemia
1.4 Pre-Transfusion Testing
- ABO grouping
- Rh typing
- Antibody screening
- Cross-matching
* Major crossmatch (recipient serum + donor RBCs)
1.5 Transfusion Procedure (Stepwise)
- Confirm indication and consent
- Verify patient identity (2 identifiers)
- Baseline vitals
- Start transfusion slowly (first 15 min)
- Monitor vitals at 15 min, hourly, post-transfusion
- Complete within:
* PRBCs: ≤4 hours
* Platelets: ≤30–60 min
* FFP: ≤2 hours
1.6 Complications of Blood Transfusion
A. Acute (≤24 hours)
1. Acute Hemolytic Transfusion Reaction (AHTR)
- Cause: ABO incompatibility
- Features: Fever, chills, back pain, hemoglobinuria, shock
- Management:
* Stop transfusion immediately
* IV fluids, maintain urine output
* Send blood and urine for hemolysis workup
2. Febrile Non-Hemolytic Reaction
- Cytokines from donor leukocytes
- Treat: Antipyretics
3. Allergic Reaction
- Urticaria → antihistamines
- Anaphylaxis (IgA deficiency) → epinephrine
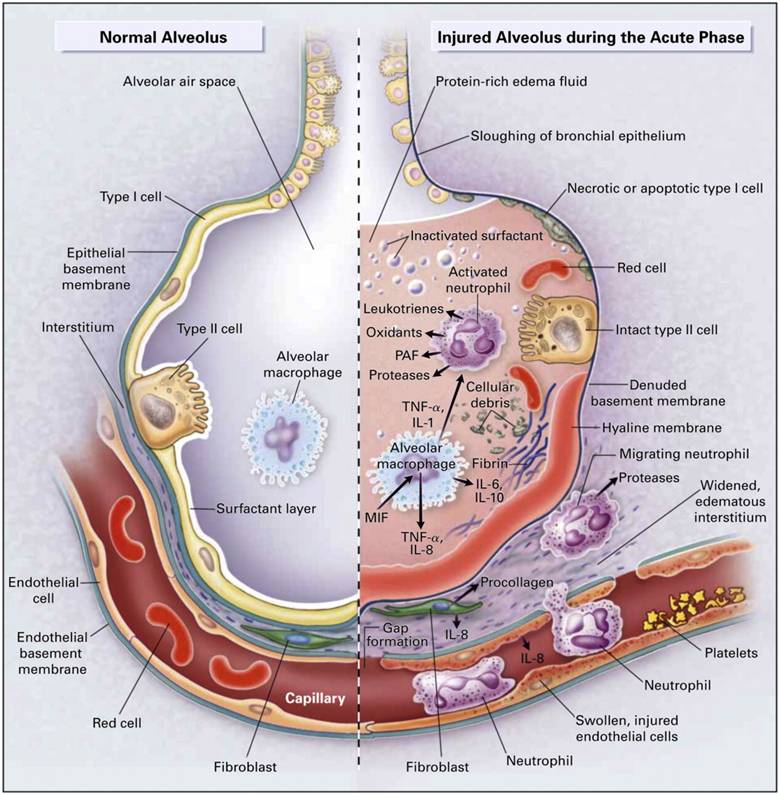
4. TRALI (Transfusion-Related Acute Lung Injury)
- Non-cardiogenic pulmonary edema
- Treat: Oxygen, ventilatory support
5. TACO (Transfusion-Associated Circulatory Overload)
- Volume overload
- Treat: Diuretics, slow transfusion
B. Delayed Complications
- Delayed hemolytic reaction
- Iron overload (chronic transfusion)
- Alloimmunization
- Transfusion-transmitted infections (HBV, HCV, HIV – rare)
1.7 Special Transfusion Situations
A. Emergency Transfusion
- Use O negative PRBCs
- Group-specific as soon as possible
B. Transfusion in Pregnancy
- Rh-negative mothers → Anti-D prophylaxis
C. Pediatric Transfusion
- Dose-based (10–15 mL/kg PRBC)
2. MASSIVE BLOOD TRANSFUSION PROTOCOL (MTP)
2.1 Definition
Massive transfusion is defined as:
- ≥10 units PRBCs in 24 hours
OR
- ≥4 units PRBCs in 1 hour with ongoing bleeding
OR
- Replacement of ≥50% blood volume in 3 hours
2.2 Indications for MTP Activation
- Major trauma with hemorrhagic shock
- Obstetric hemorrhage (PPH)
- GI bleeding with shock
- Major surgery with uncontrolled bleeding
- Ruptured aneurysm
2.3 Goals of MTP
- Restore oxygen delivery
- Prevent coagulopathy
- Avoid hypothermia, acidosis, hypocalcemia
(Lethal Triad)
2.4 MTP Blood Component Ratio
Balanced Transfusion Strategy (Damage Control Resuscitation)
| Component | Ratio |
| ------------ | ----- |
| PRBCs | 1 |
| Plasma (FFP) | 1 |
| Platelets | 1 |
➡ 1:1:1 ratio
2.5 Standard MTP Pack (Example)
Pack 1
- 4 PRBCs
- 4 FFP
- 1 platelet unit
Pack 2
- Repeat + cryoprecipitate (if fibrinogen low)
2.6 Laboratory Monitoring During MTP
- Hb/Hct
- Platelet count
- INR/PT/aPTT
- Fibrinogen
- ABG (pH, lactate)
- Ionized calcium
- Core temperature
(Prefer viscoelastic testing: TEG/ROTEM if available)
2.7 Adjunctive Therapies in MTP
A. Tranexamic Acid (TXA)
- Indication: Trauma with hemorrhage within 3 hours
- Dose:
* 1 g IV over 10 min
* Then 1 g over 8 hours
B. Calcium Replacement
- Citrate toxicity → hypocalcemia
- Give:
* Calcium gluconate 10 mL IV
* Or calcium chloride (central line)
C. Warming Measures
- Blood warmers
- Forced air warming blankets
2.8 Complications of Massive Transfusion
| Complication | Mechanism |
| ----------------------- | ------------------- |
| Dilutional coagulopathy | Factor dilution |
| Hypocalcemia | Citrate binding |
| Hypothermia | Cold blood |
| Metabolic acidosis | Shock, lactate |
| Hyperkalemia | Stored RBCs |
| ARDS | TRALI, inflammation |
2.9 Stopping Criteria for MTP
- Hemodynamic stability
- Controlled bleeding
- Normalizing coagulation profile
- Reduced transfusion requirement
3. COMPARISON: ROUTINE VS MASSIVE TRANSFUSION
| Feature | Routine | Massive |
| ---------- | ------------------ | ---------------------------- |
| Indication | Anemia/bleeding | Life-threatening hemorrhage |
| Ratio | Component-specific | 1:1:1 |
| Monitoring | Intermittent | Continuous |
| Adjuncts | Rare | TXA, calcium |
| Risk | Lower | High metabolic complications |
4. KEY EXAM & CLINICAL PEARLS
- Hb threshold alone should not dictate transfusion in shock
- Early plasma and platelets reduce mortality in trauma
- Hypocalcemia is common and often overlooked in MTP
- Always suspect TRALI vs TACO in post-transfusion respiratory distress
- Transfusion is a treatment with risks, not benign fluid
5. SUMMARY
- Blood transfusion should be indication-driven and component-specific
- Massive transfusion requires early, balanced, protocol-based resuscitation
- Continuous monitoring and complication prevention are critical
- Proper protocols save lives in trauma, obstetrics, and surgery