Aortic Stenosis (AS)
Definition
Aortic stenosis is fixed obstruction to left ventricular (LV) outflow at the level of the aortic valve (most commonly), leading to pressure overload, LV hypertrophy, and (when advanced) reduced cardiac output and heart failure. ([AHA Journals][1])
Pathophysiology (What’s happening)
- Valve narrowing → LV must generate higher systolic pressure to eject blood.
- Concentric LV hypertrophy develops → initially preserves EF but causes:
* Diastolic dysfunction (stiff LV → ↑ LVEDP → pulmonary congestion)
* Subendocardial ischemia (↑ wall stress, reduced coronary reserve) even without CAD
- Late stage: LV decompensation → falling EF, low-flow state, pulmonary HTN, TR/MR may worsen. ([AHA Journals][1])
Etiology / Causes
Common
- Degenerative calcific AS (older adults) — most common in high-income settings
- Bicuspid aortic valve (earlier onset; associated with aortopathy)
- Rheumatic AS (often mixed AS + AR; more common in endemic areas)
Less common
- Congenital unicuspid valve, radiation-related, CKD/mineral bone disease, Paget disease. ([AHA Journals][1])
Severity Grading (Key Echo Criteria)
High-gradient severe AS is typically:
- Peak velocity (Vmax) ≥ 4.0 m/s and/or mean gradient ≥ 40 mmHg, and
- Aortic valve area (AVA) ≤ 1.0 cm² (indexed AVA ≤ 0.6 cm²/m² often used). ([eurointervention.pcronline.com][2])
Important “discordant” severe AS phenotypes
- Low-flow, low-gradient severe AS with reduced EF
- Paradoxical low-flow, low-gradient severe AS with preserved EF
- Normal-flow, low-gradient (measurement/systemic factors)
These often need dobutamine stress echo and/or CT aortic valve calcium to confirm severity. ([uptodate.com][3])
Clinical Features
Classic symptoms (often late; high risk once present)
- Angina
- Syncope/presyncope (exertional)
- Dyspnea / heart failure symptoms (orthopnea, PND, edema)
Other symptoms
- Reduced exercise tolerance, fatigue, palpitations, sudden cardiac death risk increases in severe symptomatic disease. ([AHA Journals][1])
Physical Examination (High-yield)
- Slow-rising, low-volume pulse (pulsus parvus et tardus)
- Narrow pulse pressure (often)
- Ejection systolic murmur at right upper sternal border radiating to carotids
- Soft/absent A2 in severe AS
- S4 (stiff LV), heaving apex, signs of HF in advanced cases
Investigations / Diagnosis
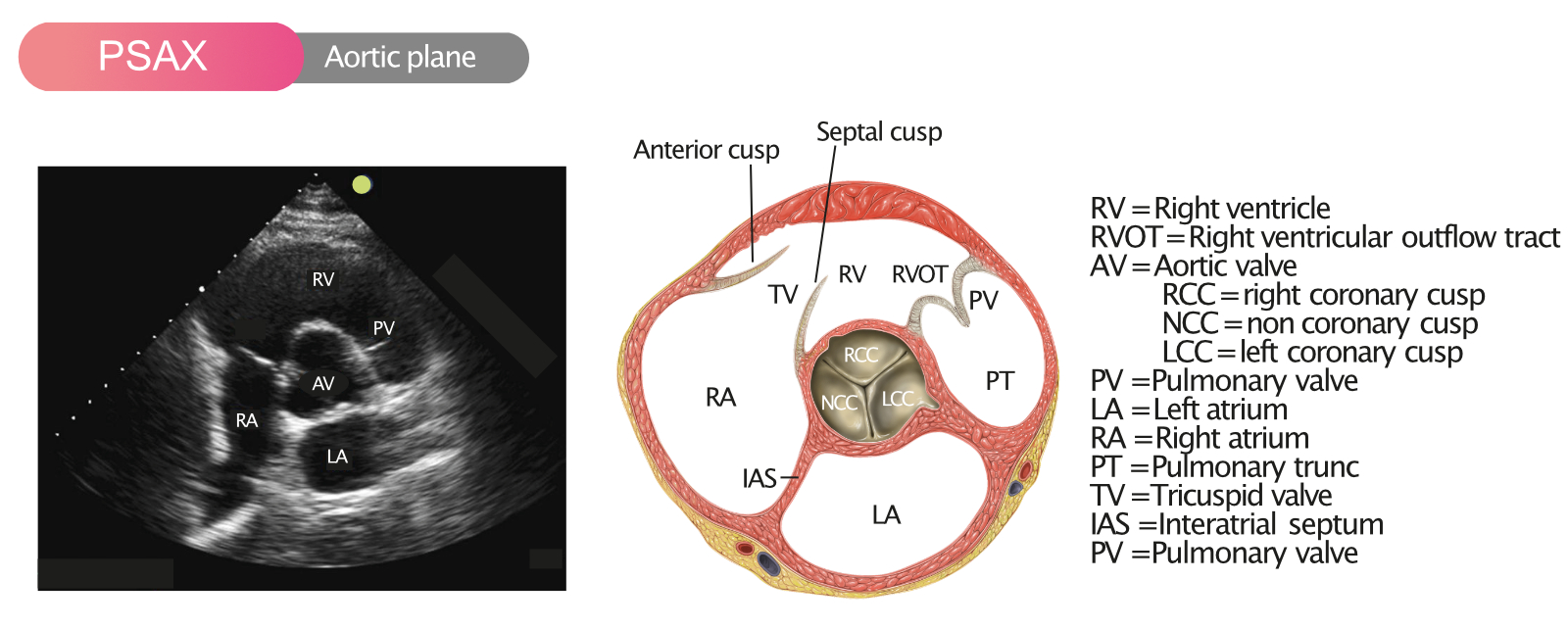
1) Transthoracic echocardiography (TTE) — cornerstone
- Vmax, mean gradient, AVA (continuity equation)
- LV size/function, hypertrophy, diastolic function
- Other valves, pulmonary pressures, aortic root/ascending aorta assessment. ([PMC][4])
2) ECG / CXR
- LVH/strain, AF; CXR may show post-stenotic dilation, congestion.
3) Stress testing (selected)
- Exercise test can unmask symptoms in “asymptomatic severe AS” (done under specialist supervision; not for symptomatic severe AS). ([AHA Journals][1])
4) Low-flow/low-gradient workup
- Low-dose dobutamine stress echo (true severe vs pseudo-severe)
- CT aortic valve calcium scoring helpful when echo discordant. ([uptodate.com][3])
5) Coronary assessment before intervention
- Coronary angiography/CT coronary as appropriate (especially before SAVR/TAVR). ([AHA Journals][1])
Differential Diagnoses
- Hypertrophic obstructive cardiomyopathy (dynamic obstruction)
- Aortic sclerosis (thickened valve without significant obstruction)
- Subaortic stenosis (membrane), supravalvular AS
- Severe hypertension causing high gradients
- Mitral regurgitation / HFpEF mimicking dyspnea causes
Management (Stepwise, Practical)
1) Immediate priorities
If symptomatic severe AS with instability
- Hospitalize, treat pulmonary edema cautiously, urgent valve-team evaluation.
- Avoid precipitous BP drops; maintain sinus rhythm/adequate preload. ([AHA Journals][1])
2) Definitive treatment (only proven life-saving therapy)
A) Aortic Valve Replacement
Indications (core principles)
- Severe AS + symptoms → valve intervention recommended (unless prohibitive) ([AHA Journals][1])
- Severe AS + LV systolic dysfunction (reduced EF attributable to AS) → intervene ([AHA Journals][1])
- Asymptomatic severe AS: intervene in selected high-risk features (examples commonly used in guidelines/valve teams):
* Very severe AS (very high Vmax/gradient)
* Abnormal exercise test (symptoms or BP drop)
* Rapid progression, markedly elevated BNP (context-dependent)
* Need for other cardiac surgery
Approach choice: SAVR vs TAVR
- Done by a multidisciplinary Heart Team considering age, surgical risk, anatomy (access, annulus, coronary heights), life expectancy, valve durability strategy, and patient preference. ([AHA Journals][1])
B) Balloon Aortic Valvuloplasty (BAV)
- Temporary/bridge in selected patients (e.g., unstable, need urgent non-cardiac surgery, bridge-to-TAVR/SAVR) or palliative when no definitive option. ([AHA Journals][1])
3) Medical therapy (supportive only — does not “cure” AS)
There is no medication that reliably stops or reverses established severe calcific AS; meds are used to treat comorbidities and symptoms carefully. ([AHA Journals][1])
Non-pharmacologic
- Avoid dehydration/excess diuresis; avoid extreme exertion in severe AS.
- Vaccination, dental hygiene (endocarditis prevention behavior).
- Manage CV risk factors (smoking cessation, lipids, BP, diabetes).
Drugs (Complete “mini-monographs” for common AS-related use)
> Doses below are typical adult starting/target ranges; tailor to BP, renal function, electrolytes, and specialist advice. Pediatric dosing is rarely applicable for typical degenerative AS; if you need congenital/pediatric AS dosing, tell me the age/weight.
1) Loop diuretic — Furosemide
- Indication in AS: Pulmonary congestion/edema or volume overload HF symptoms with caution (risk: preload reduction → hypotension/syncope).
- MOA: Inhibits NKCC2 in thick ascending limb → natriuresis/diuresis.
- Usual dosing (adult):
* Chronic congestion: 20–40 mg PO once daily, titrate.
* Acute pulmonary edema: 20–80 mg IV, repeat/titrate.
- PK: Onset IV minutes; oral 30–60 min. Renal excretion; reduced effect in CKD (needs higher doses).
- Adverse effects:
* Common: hypokalemia, hyponatremia, dehydration, gout, hypotension
* Serious: ototoxicity (high IV dose), renal dysfunction
- Contraindications: Anuria; severe sulfonamide allergy is relative.
- Interactions: NSAIDs reduce effect; digoxin toxicity risk ↑ with hypokalemia; aminoglycosides ↑ ototoxicity.
- Monitoring: BP, weight, urine output, K/Na/Mg, creatinine.
- Counselling: Take earlier in day; stand up slowly; report dizziness, cramps, hearing changes.
2) ACE inhibitor — Enalapril (or similar ACEi)
- Indication in AS: Hypertension and HF when needed, especially if coexistent LV dysfunction; start low, monitor closely (severe symptomatic AS can be preload/afterload sensitive).
- MOA: ↓ Angiotensin II, ↓ aldosterone → vasodilation, natriuresis.
- Usual dosing (adult): 2.5–5 mg PO daily, titrate (often to 10–20 mg/day in divided doses depending on goal/tolerance).
- PK: Prodrug → enalaprilat; renal elimination.
- Adverse effects: cough, hyperkalemia, creatinine rise, dizziness; rare angioedema.
- Contraindications: Pregnancy, history of ACEi angioedema, bilateral renal artery stenosis.
- Interactions: K supplements/spironolactone ↑ hyperkalemia; NSAIDs ↑ renal risk; lithium ↑ levels.
- Monitoring: BP, creatinine/eGFR, K within 1–2 weeks after start/titration.
- Counselling: Report facial swelling; avoid salt substitutes (potassium).
3) ARB — Losartan (if ACEi not tolerated)
- Indication: Same as ACEi (HTN/HF), ACEi cough intolerance.
- MOA: AT1 receptor blockade.
- Dose: 25–50 mg PO daily, titrate to 100 mg/day.
- PK: Hepatic metabolism; active metabolite.
- Adverse effects: hyperkalemia, renal function change, dizziness; angioedema rare.
- Contraindications/Monitoring/Interactions: Similar to ACEi (no cough).
4) Beta-blocker — Metoprolol (succinate or tartrate)
- Indication in AS: Rate control (AF), angina/CAD, HF with reduced EF (specialist-guided). Use cautiously if severe symptomatic AS with low output.
- MOA: β1 blockade → ↓ HR, ↓ myocardial oxygen demand.
- Dose:
* Tartrate: 25–50 mg PO twice daily (start lower if frail)
* Succinate: 12.5–25 mg PO daily, titrate.
- PK: Hepatic metabolism (CYP2D6).
- Adverse effects: bradycardia, hypotension, fatigue, bronchospasm (less with β1 selective), worsening HF if started too aggressively.
- Contraindications: severe bradycardia, 2nd/3rd degree AV block (no pacer), cardiogenic shock.
- Interactions: verapamil/diltiazem ↑ bradycardia/AV block; other negative chronotropes.
- Monitoring: HR, BP, symptoms; ECG in conduction disease.
- Counselling: Don’t stop abruptly; watch for dizziness, wheeze, very slow pulse.
5) Anticoagulation for AF (common in AS) — Apixaban (example DOAC)
- Indication: Stroke prevention in non-valvular AF (AS counts as “non-valvular” in DOAC terminology; exceptions include mechanical valves and moderate–severe rheumatic mitral stenosis). ([American College of Cardiology][5])
- MOA: Direct factor Xa inhibitor.
- Dose (adult): 5 mg PO twice daily; reduce to 2.5 mg BID if patient meets standard dose-reduction criteria (age/weight/creatinine criteria per label/local guidance).
- PK: Mixed renal/hepatic clearance.
- Adverse effects: bleeding, bruising; rare hepatic issues.
- Contraindications: active major bleeding; severe hypersensitivity; caution severe renal/liver disease.
- Interactions: strong CYP3A4/P-gp inhibitors/inducers affect levels.
- Monitoring: renal function periodically; bleeding signs.
- Counselling: adherence is critical; report bleeding, black stools; tell providers before procedures.
(If you want, tell me the patient’s age/creatinine/weight and I’ll compute the correct DOAC dose rules precisely.)
Follow-up & Surveillance (typical approach)
- Repeat echo interval depends on severity (more frequent as severity increases).
- Prompt reassessment if new symptoms, syncope, HF signs, or change in murmur. ([AHA Journals][1])
Complications
- Heart failure, pulmonary hypertension
- Arrhythmias (AF, ventricular ectopy), syncope, sudden cardiac death (risk highest once symptomatic)
- GI angiodysplasia bleeding (Heyde syndrome), endocarditis
- Progressive LV dysfunction and irreversible myocardial fibrosis if intervention delayed. ([AHA Journals][1])
Red Flags (urgent evaluation)
- New exertional syncope
- Rest dyspnea/pulmonary edema
- Chest pain at rest
- Hypotension/low output signs
- New AF with HF symptoms
External links (authoritative) — copy/paste
`text
ACC/AHA 2020 Valvular Heart Disease Guideline (AHA journal page):
https://www.ahajournals.org/doi/10.1161/CIR.0000000000000923
ACC “Guidelines Made Simple” (PDF summary tool):
https://www.acc.org/-/media/Non-Clinical/Files-PDFs-Excel-MS-Word-etc/Guidelines/2020/VHD-Guidelines-Made-Simple-Tool-gl-vhd.pdf
2021 ESC/EACTS Valvular Heart Disease Guidelines (EuroIntervention):
https://eurointervention.pcronline.com/article/2021-esc-eacts-guidelines-for-the-management-of-valvular-heart-disease
ESC Guideline hub (Valvular Heart Disease; includes updates):
https://www.escardio.org/Guidelines/Clinical-Practice-Guidelines/Valvular-Heart-Disease
Open-access practical echo assessment review (PMC):
https://pmc.ncbi.nlm.nih.gov/articles/PMC8115410/
NICE Interventional Guidance on TAVI (IPG586):
https://www.nice.org.uk/guidance/ipg586
`
If you want, tell me age, symptoms, echo values (Vmax/mean gradient/AVA), EF, and BP—and I’ll convert this into a decision-ready plan (severity category + what to do next + which tests to confirm if discordant).
[1]: https://www.ahajournals.org/doi/10.1161/CIR.0000000000000923?utm_source=chatgpt.com "2020 ACC/AHA Guideline for the Management of Patients ..."
[2]: https://eurointervention.pcronline.com/article/2021-esc-eacts-guidelines-for-the-management-of-valvular-heart-disease?utm_source=chatgpt.com "2021 ESC/EACTS Guidelines for the management of ..."
[3]: https://www.uptodate.com/contents/low-gradient-severe-aortic-stenosis-clinical-manifestations-and-diagnosis?utm_source=chatgpt.com "Low gradient severe aortic stenosis"
[4]: https://pmc.ncbi.nlm.nih.gov/articles/PMC8115410/?utm_source=chatgpt.com "Echocardiographic assessment of aortic stenosis: a practical ..."
[5]: https://www.acc.org/-/media/Non-Clinical/Files-PDFs-Excel-MS-Word-etc/Guidelines/2020/VHD-Guidelines-Made-Simple-Tool-gl-vhd.pdf?utm_source=chatgpt.com "2020 Guideline for the Management of Patients With ..."
Below are 20 detailed, exam-oriented clinical case scenarios on Aortic Stenosis, each written as a complete vignette with interpretation and management, suitable for UG/PG exams, OSCEs, ward teaching, and clinical reasoning practice.
1. Exertional Syncope in Elderly
Scenario:
A 74-year-old man collapses while climbing stairs. He has a harsh ejection systolic murmur radiating to the carotids and a slow-rising pulse. BP 130/80 mmHg.
Interpretation:
Symptomatic severe aortic stenosis causing fixed cardiac output and cerebral hypoperfusion.
Management:
Urgent echocardiography → confirm severe AS → aortic valve replacement (TAVR/SAVR).
2. Angina With Normal Coronary Arteries
Scenario:
A 68-year-old woman has exertional chest pain. Coronary angiography is normal. Echo shows concentric LVH and AVA 0.8 cm².
Interpretation:
Subendocardial ischemia due to LV hypertrophy in severe AS.
Management:
Definitive AVR, avoid relying on anti-anginal drugs alone.
3. Acute Pulmonary Edema in Critical AS
Scenario:
A 70-year-old man presents with acute pulmonary edema. BP 95/60 mmHg, loud systolic murmur, soft A2.
Interpretation:
Critical AS with diastolic dysfunction.
Management:
Oxygen, cautious low-dose diuretics, avoid aggressive vasodilators → urgent valve intervention.
4. Asymptomatic Severe AS With Abnormal Stress Test
Scenario:
A 62-year-old man denies symptoms. Echo: AVA 0.7 cm². Exercise test causes dyspnea and hypotension.
Interpretation:
High-risk asymptomatic severe AS.
Management:
Early aortic valve replacement.
5. Low-Flow Low-Gradient AS With Reduced EF
Scenario:
A 66-year-old man has dyspnea, EF 30%, AVA 0.9 cm², gradient 28 mmHg.
Interpretation:
Low-flow low-gradient AS.
Management:
Low-dose dobutamine stress echo → confirm true severe AS → AVR.
6. Paradoxical Low-Flow AS With Preserved EF
Scenario:
A 73-year-old woman has exertional dyspnea, EF 60%, small hypertrophied LV, low gradient.
Interpretation:
Paradoxical low-flow severe AS due to diastolic dysfunction.
Management:
CT valve calcium scoring → AVR if severe confirmed.
7. Bicuspid Aortic Valve in Middle Age
Scenario:
A 48-year-old man has a systolic murmur. Echo shows bicuspid valve with moderate AS.
Interpretation:
Congenital AS with risk of aortopathy.
Management:
Serial echo + CT/MRI of ascending aorta, lifestyle advice.
8. Atrial Fibrillation Precipitating Heart Failure
Scenario:
A patient with known AS develops sudden AF with rapid ventricular response and pulmonary edema.
Interpretation:
Loss of atrial kick in stiff LV.
Management:
Urgent rate/rhythm control, anticoagulation → plan AVR.
9. Heyde Syndrome
Scenario:
An elderly man with severe AS has recurrent iron-deficiency anemia and GI bleeding.
Interpretation:
Heyde syndrome (AS + GI angiodysplasia + acquired vWF deficiency).
Management:
Definitive treatment is aortic valve replacement.
10. Sudden Cardiac Death Risk
Scenario:
A 69-year-old man with severe AS collapses suddenly at home.
Interpretation:
Malignant ventricular arrhythmia in severe AS.
Management:
Prevention is early valve replacement once symptomatic.
11. Preoperative Evaluation for Non-Cardiac Surgery
Scenario:
A 71-year-old woman with severe AS requires urgent abdominal surgery.
Interpretation:
High perioperative risk due to fixed outflow obstruction.
Management:
Optimize hemodynamics, consider BAV or TAVR before surgery if feasible.
12. Hypertension in Aortic Stenosis
Scenario:
A patient with moderate AS has uncontrolled hypertension.
Interpretation:
Afterload increases LV stress.
Management:
Careful BP control with low-dose ACEi/ARB, close monitoring.
13. Progressive Murmur in Elderly
Scenario:
A 76-year-old woman has increasing murmur intensity over 2 years.
Interpretation:
Progressive calcific AS.
Management:
Repeat echocardiography → monitor progression → intervene when severe/symptomatic.
14. Rheumatic Aortic Stenosis
Scenario:
A 60-year-old woman has AS with associated mitral stenosis.
Interpretation:
Rheumatic heart disease.
Management:
Evaluate both valves → combined valve surgery if indicated.
15. Reduced Exercise Tolerance Only
Scenario:
A patient reports reduced walking capacity but no chest pain or syncope.
Interpretation:
Early symptom of AS often under-reported.
Management:
Treat as symptomatic severe AS → AVR.
16. New Left Bundle Branch Block After TAVR
Scenario:
Post-TAVR patient develops LBBB on ECG.
Interpretation:
Conduction system injury.
Management:
Continuous monitoring, pacemaker if high-grade AV block develops.
17. Pregnancy With Moderate AS
Scenario:
A pregnant woman has known moderate AS and mild dyspnea.
Interpretation:
Increased circulatory demand.
Management:
Conservative management, close monitoring, avoid hypotension.
18. Elderly Frail Patient With Severe AS
Scenario:
An 85-year-old frail woman with severe AS and multiple comorbidities.
Interpretation:
High surgical risk.
Management:
TAVR preferred after heart-team evaluation.
19. Elevated BNP in Asymptomatic AS
Scenario:
Asymptomatic patient with severe AS has markedly elevated BNP.
Interpretation:
Subclinical myocardial decompensation.
Management:
Consider early valve replacement.
20. Medical Therapy Alone in Severe AS
Scenario:
A patient refuses surgery and is treated medically.
Interpretation:
Poor long-term prognosis.
Management:
Symptom palliation, patient counseling, revisit definitive intervention options.