BREASTFEEDING AND BREAST MILK (PEDIATRICS) — COMPLETE DETAIL
1. Definition
Breastfeeding
Breastfeeding is the process of feeding an infant with milk produced by the mother’s mammary glands.
Exclusive Breastfeeding (EBF)
Infant receives only breast milk (no water, formula, or other foods) except medicines/vitamins.
✅ Recommended for the first 6 months of life.
2. Physiology of Lactation
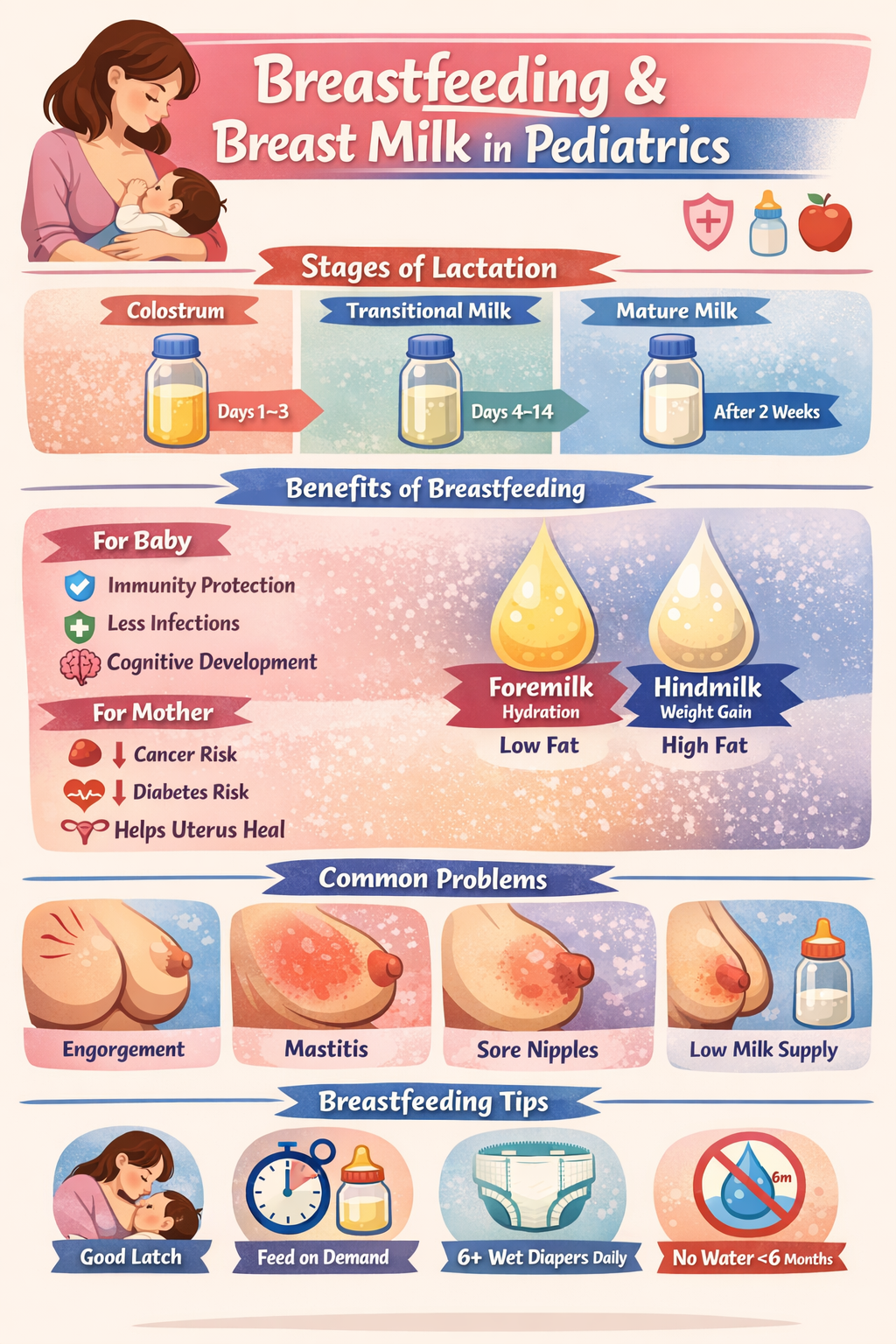
Stages of Lactation
Stage I: Lactogenesis I (Mid-pregnancy)
- Breast tissue develops
- Colostrum production begins
Stage II: Lactogenesis II (2–4 days postpartum)
- “Milk comes in”
- Triggered by:
* Delivery of placenta → ↓ progesterone
* ↑ prolactin effect
Stage III: Galactopoiesis (Maintenance phase)
- Milk production maintained by:
* Frequent suckling
* Effective emptying of breast
3. Hormonal Control
Prolactin
- Produced by anterior pituitary
- Responsible for milk production
Oxytocin
- Produced by posterior pituitary
- Causes milk ejection reflex (let-down)
Inhibitors
- Stress, pain, anxiety → ↓ oxytocin → poor let-down
4. Composition of Breast Milk
Breast milk is a dynamic living fluid.
Colostrum (Days 1–3)
- Thick, yellow
- Small quantity but very concentrated
Contains:
- High IgA
- Lactoferrin
- Leukocytes
- Growth factors
✅ Acts as the baby’s first vaccine
Transitional Milk (Day 4–14)
- Increased volume
- More fat and lactose
Mature Milk (After 2 weeks)
Components:
- Water: 87%
- Carbohydrates: Lactose (main energy source)
- Fats: Essential fatty acids, DHA
- Proteins: Whey > Casein (easy digestion)
- Immune factors: IgA, lysozyme
- Cells: Macrophages, lymphocytes
5. Foremilk vs Hindmilk
| Feature | Foremilk | Hindmilk |
| ---------------- | -------------------- | ------------------- |
| At start of feed | Yes | Later |
| Composition | More water + lactose | More fat + calories |
| Function | Hydration | Weight gain |
6. Benefits of Breastfeeding
A. Benefits for Infant
Nutritional
- Perfect balance of nutrients
- Easily digestible
Immunological Protection
Reduces:
- Diarrhea
- Pneumonia
- Otitis media
- Meningitis
- Neonatal sepsis
Long-term Benefits
Lower risk of:
- Obesity
- Type 1 & Type 2 diabetes
- Asthma/allergy
- Childhood leukemia
Neurodevelopment
- Improved IQ and cognitive outcomes
B. Benefits for Mother
- Helps uterine involution (oxytocin effect)
- Decreases postpartum hemorrhage
- Lactational amenorrhea (natural spacing)
- Reduced risk of:
* Breast cancer
* Ovarian cancer
* Type 2 diabetes
7. WHO & AAP Recommendations
- Initiate breastfeeding within 1 hour of birth
- Exclusive breastfeeding for 6 months
- Continue breastfeeding with complementary foods up to:
* 2 years or beyond
8. Technique of Breastfeeding
Proper Positioning
- Baby’s head and body aligned
- Baby facing breast
- Full body supported
Proper Latch (Attachment)
Signs of good latch:
- Mouth wide open
- Chin touching breast
- More areola visible above than below
- No pain
- Audible swallowing
9. Feeding Frequency
- Newborn feeds 8–12 times/day
- Feed on demand, not clock-based
Signs baby is hungry:
- Rooting
- Hand-to-mouth movements
- Lip smacking
Crying = late sign
10. Indicators of Adequate Milk Intake
By Day 5:
- ≥6 wet diapers/day
- ≥3 stools/day (yellow)
- Weight gain begins after initial loss
Normal weight loss:
- Up to 7–10% in first week
11. Common Breastfeeding Problems
A. Poor Latch
Causes:
- Incorrect positioning
- Flat/inverted nipple
Management:
- Correct technique
- Lactation support
B. Breast Engorgement
- Painful, swollen breasts
Treatment:
- Frequent feeding
- Warm compress before feeding
- Cold compress after feeding
C. Cracked/Sore Nipples
Cause: poor latch
Treatment:
- Improve latch
- Apply expressed breast milk
- Lanolin cream
D. Mastitis
Symptoms:
- Fever
- Breast redness, pain
Treatment:
- Continue breastfeeding
- Antibiotics:
* Dicloxacillin
* Cephalexin
E. Breast Abscess
- Fluctuant swelling
Management:
- Drainage + antibiotics
F. Low Milk Supply
Usually due to:
- Infrequent feeding
- Poor latch
Management:
- Increase feeds
- Pumping
- Maternal hydration/nutrition
12. Contraindications to Breastfeeding
Absolute Contraindications
Infant:
- Classic galactosemia
Mother:
- HIV infection (in high-resource settings)
- Active untreated TB (temporary)
- HTLV-1/2 infection
- Chemotherapy drugs
Relative Contraindications
- Certain medications (radioactive iodine)
- Herpes lesions on breast (avoid affected side)
13. Breastfeeding in Special Situations
Preterm Infants
- Breast milk reduces NEC risk
- Fortification may be needed
Twins
- Possible with proper support
Working Mothers
- Expressed breast milk storage
14. Expressed Breast Milk Storage Guidelines
| Location | Duration |
| ------------------ | -------- |
| Room temp (25°C) | 4 hours |
| Refrigerator (4°C) | 4 days |
| Freezer (-18°C) | 6 months |
Thawing:
- Warm water bath
- Do NOT microwave
15. Complementary Feeding After 6 Months
Continue breastfeeding + introduce:
- Iron-rich foods
- Fruits, vegetables
- Protein sources
Breastfeeding remains major nutrition up to 1 year.
16. Lactational Amenorrhea Method (LAM)
Effective contraception if:
- Baby <6 months
- Exclusive breastfeeding
- Mother amenorrheic
Effectiveness: ~98%
17. Key Counseling Points for Parents
- Breastfeeding is best nutrition for infant
- Feed on demand
- Correct latch prevents pain
- No water needed in first 6 months
- Seek help early for problems
- Continue breastfeeding during mild illness
Quick Pediatric Exam Notes
- Colostrum = rich in IgA
- Exclusive breastfeeding = 6 months
- Breast milk protects against infection + obesity
- Foremilk hydrates, hindmilk fattens
- Mastitis: continue feeding + antibiotics