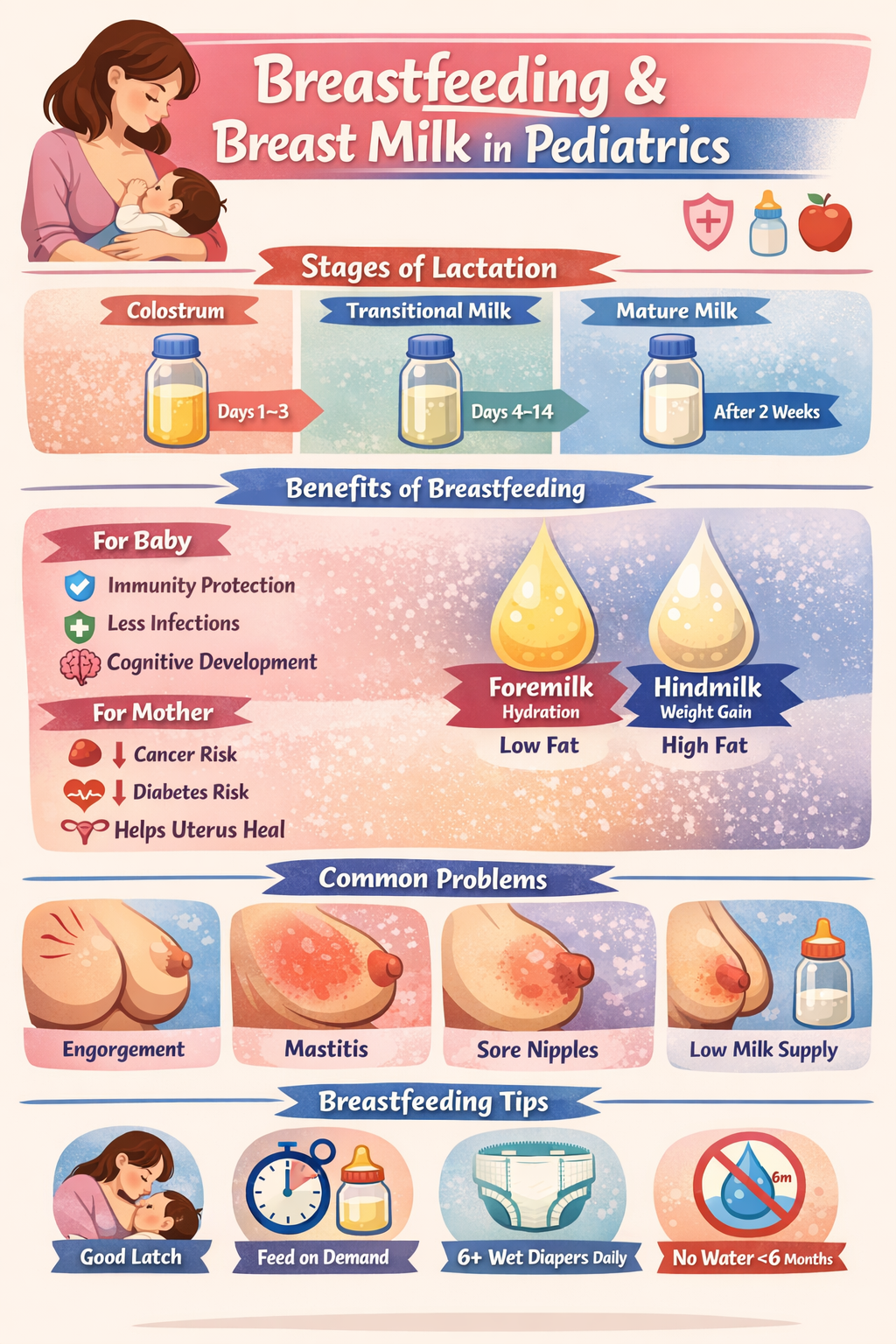
Breastfeeding in Paediatrics (Complete Overview)
1. Definition
Breastfeeding is the process of feeding an infant with milk directly from the mother’s breast. It provides optimal nutrition and immunological protection for newborns and infants and is considered the gold standard for infant feeding.
2. Physiology of Lactation
Lactogenesis (Stages)
- Lactogenesis I (Secretory Differentiation)
* Begins during pregnancy (around 16–20 weeks gestation)
* Mammary glands start producing colostrum
* High progesterone prevents full milk secretion.
- Lactogenesis II (Secretory Activation)
* Occurs 2–4 days after delivery
* Triggered by drop in progesterone after placenta delivery
* Rapid increase in milk production.
- Lactogenesis III (Galactopoiesis)
* Maintenance of milk production
* Controlled by prolactin and frequent suckling.
Hormonal Regulation
Prolactin
- Produced by anterior pituitary
- Stimulates milk production in alveolar cells
- Levels increase with infant suckling
Oxytocin
- Produced by posterior pituitary
- Causes milk ejection reflex (let-down reflex)
- Triggered by infant suckling, infant cry, emotional bonding.
3. Composition of Breast Milk
Colostrum (First 3–5 days)
Characteristics:
- Thick, yellowish
- High in proteins and antibodies
Components:
- IgA
- Lactoferrin
- Leukocytes
- Growth factors
- Low fat and lactose
Functions:
- Protects against infection
- Promotes gut maturation
- Acts as natural laxative (prevents meconium retention).
Transitional Milk
- Produced 5–14 days postpartum
- Increased fat and lactose
Mature Milk
Two components:
Foremilk
- Thin
- High lactose
- Quenches thirst
Hindmilk
- Thick
- High fat
- Provides energy and satiety
4. Nutritional Composition
Breast milk contains:
Macronutrients
- Proteins: whey > casein (easily digestible)
- Fat: essential fatty acids, DHA
- Carbohydrates: lactose
Micronutrients
- Vitamins A, E, K
- Minerals: calcium, phosphorus, iron (high absorption)
Bioactive components
- Immunoglobulin A
- Lactoferrin
- Lysozyme
- Oligosaccharides (gut microbiota development)
5. Benefits of Breastfeeding
Benefits to the Infant
Nutritional
- Ideal nutrient balance
- Easily digestible
Immunological
- Reduced risk of:
* Diarrhea
* Respiratory infections
* Otitis media
* Sepsis
Long-term benefits
- Reduced risk of:
* Obesity
* Type 1 diabetes
* Type 2 diabetes
* Asthma
* Allergies
Neurodevelopment
- Improved IQ and cognitive development.
Benefits to the Mother
- Promotes uterine involution
- Reduces postpartum hemorrhage
- Natural birth spacing (lactational amenorrhea)
- Reduces risk of:
* Breast cancer
* Ovarian cancer
* Type 2 diabetes
- Helps postpartum weight loss
- Strengthens maternal-infant bonding.
6. Exclusive Breastfeeding
Definition:
Infant receives only breast milk for the first 6 months, with no additional food or drink (except medicines or vitamins).
Recommended by:
- WHO
- UNICEF
- American Academy of Pediatrics.
After 6 months, complementary feeding begins while breastfeeding continues up to 2 years or beyond.
7. Breastfeeding Technique
Proper Positioning
Mother should be comfortable and relaxed.
Common positions:
- Cradle hold
- Cross-cradle hold
- Football hold
- Side-lying position
Correct Latch
Signs of proper latch:
- Infant mouth wide open
- Lips flanged outward
- More areola visible above than below
- Chin touching breast
- No nipple pain
Signs of poor latch:
- Clicking sounds
- Nipple pain
- Infant unsatisfied.
8. Feeding Frequency
- Newborn feeds 8–12 times per day
- Feeding every 2–3 hours
- Night feeding is important for prolactin stimulation.
Signs infant is receiving adequate milk:
- Weight gain after day 10
- 6–8 wet diapers per day
- Regular stools.
9. Contraindications to Breastfeeding
Absolute Contraindications
Maternal conditions:
- HIV infection (depending on guidelines)
- Active untreated tuberculosis
- Ebola infection
Infant conditions:
- Galactosemia
Relative Contraindications
- Certain maternal medications
- Chemotherapy
- Radioactive drugs
- Herpes lesions on breast.
10. Common Breastfeeding Problems
1. Engorgement
Breast becomes swollen and painful.
Management:
- Frequent feeding
- Warm compress
- Gentle breast massage.
2. Cracked Nipples
Caused by poor latch.
Management:
- Correct positioning
- Apply breast milk to nipple
- Use nipple cream (lanolin).
3. Mastitis
Breast infection.
Symptoms:
- Pain
- Redness
- Fever
Management:
- Continue breastfeeding
- Antibiotics if bacterial.
4. Low Milk Supply
Causes:
- Infrequent feeding
- Poor latch
- Maternal stress
Management:
- Increase feeding frequency
- Ensure proper latch
- Adequate maternal nutrition.
11. Lactational Amenorrhea Method (LAM)
Breastfeeding can act as natural contraception when:
Conditions:
- Exclusive breastfeeding
- Infant age < 6 months
- Amenorrhea present
Effectiveness: ≈98%
12. Storage of Expressed Breast Milk
| Storage Location | Duration |
| ---------------- | -------- |
| Room temperature | 4 hours |
| Refrigerator | 4 days |
| Freezer | 6 months |
Before feeding:
- Warm in lukewarm water
- Do not microwave.
13. Complementary Feeding with Breastfeeding
Start at 6 months.
Foods introduced gradually:
- Cereals
- Fruits
- Vegetables
- Pulses
- Eggs
Breastfeeding should continue until 2 years or longer.
14. WHO Breastfeeding Recommendations
- Initiate breastfeeding within 1 hour of birth
- Exclusive breastfeeding for 6 months
- Continue breastfeeding for 2 years or more
- Introduce safe complementary foods after 6 months.
15. Key Paediatric Points
- Colostrum is first immunization
- Exclusive breastfeeding prevents infant mortality
- Improves growth, immunity, and neurodevelopment
- Promotes maternal and child health.
If you want, I can also provide:
- MCQs on breastfeeding for paediatrics exams
- OSCE viva questions for paediatrics
- Clinical case scenarios for medical exams.