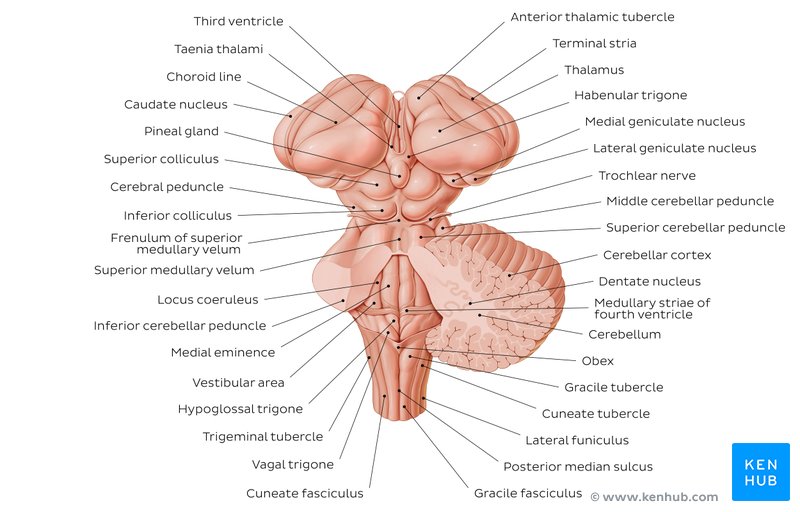
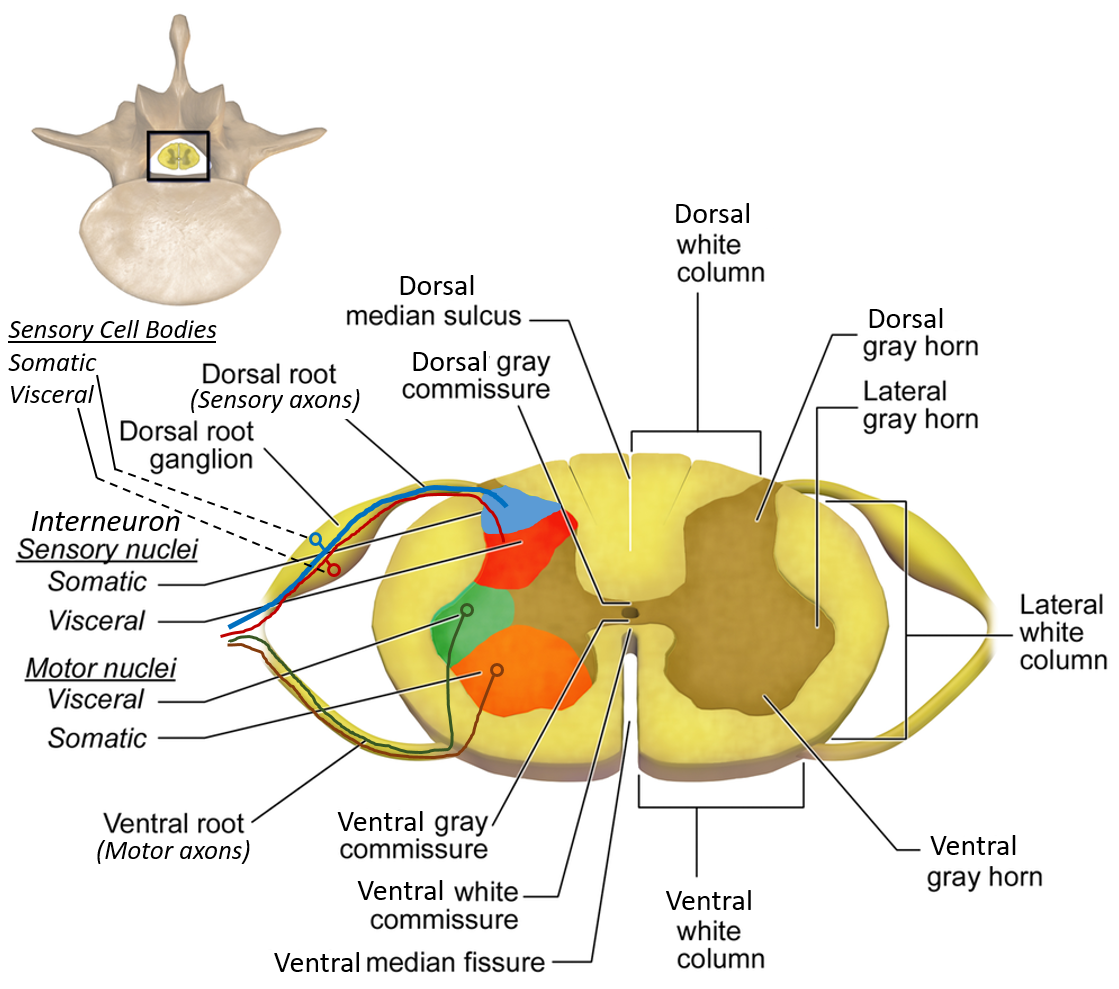
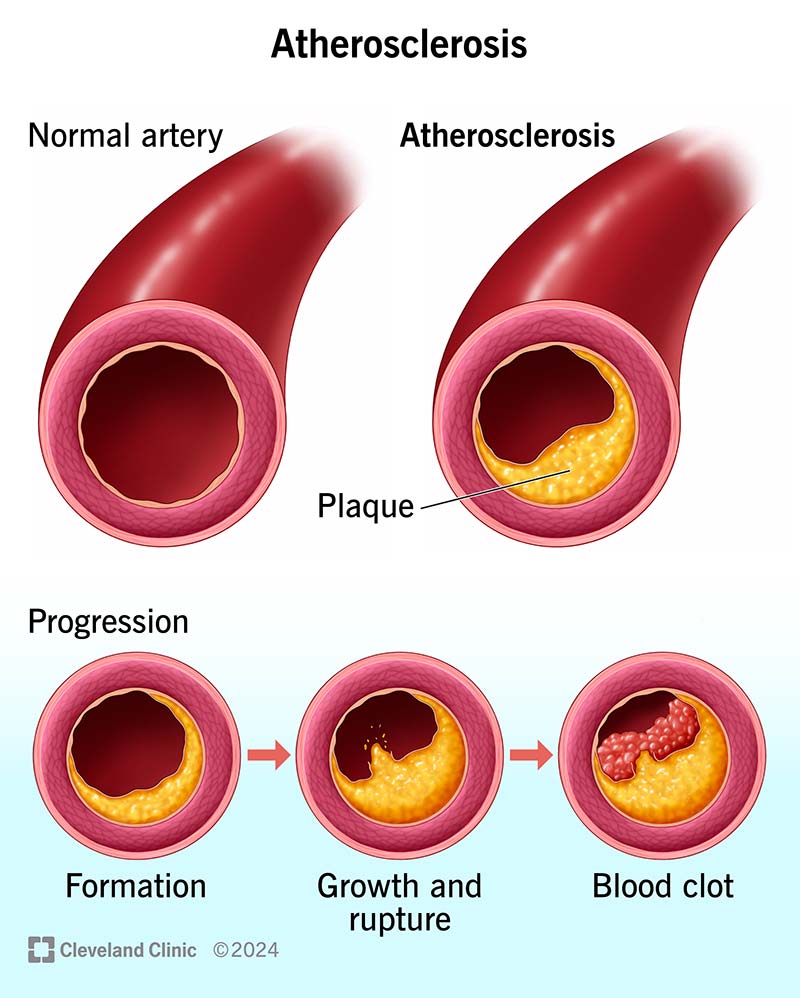
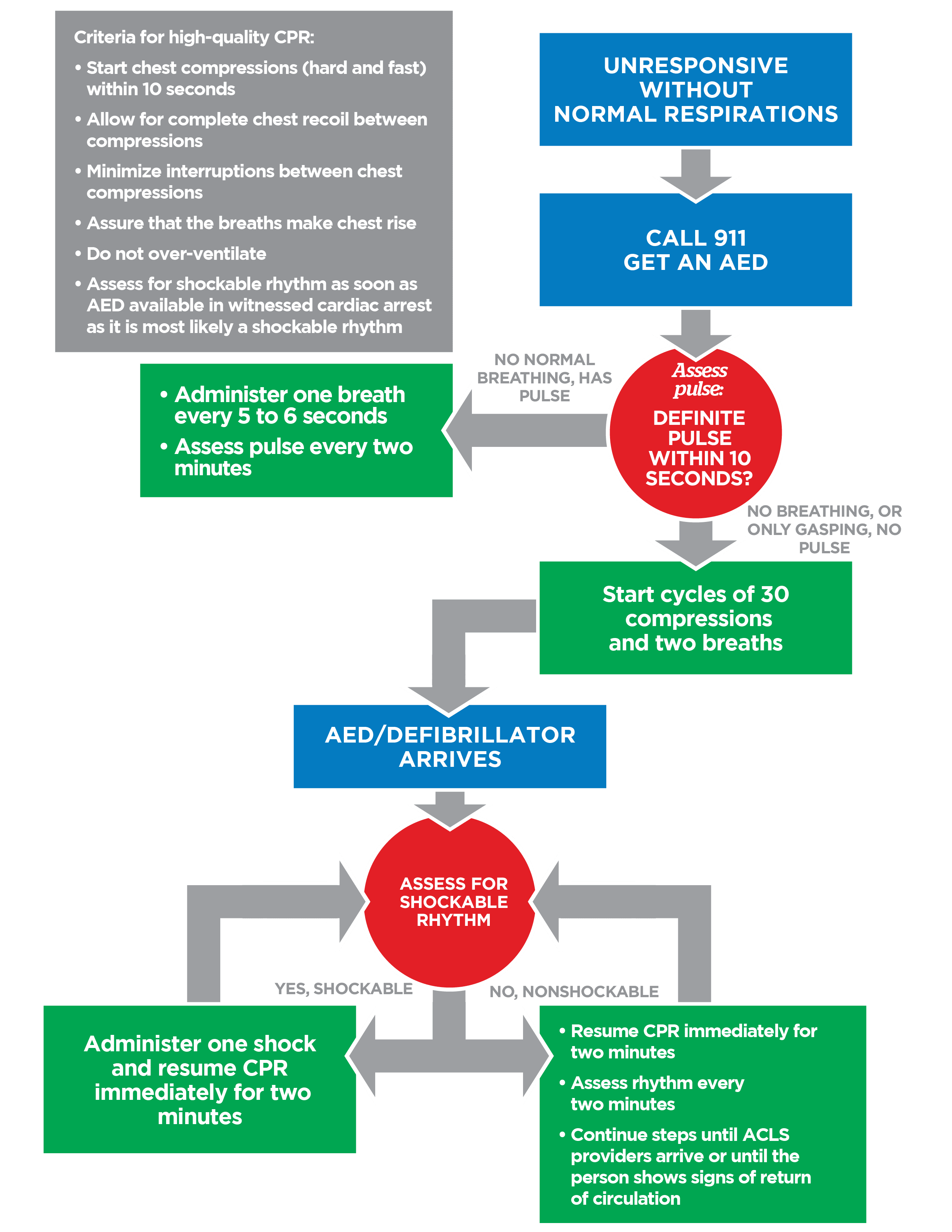
MIDBRAIN SYNDROMES
1. Weber Syndrome
Case Scenario:
A 55-year-old man presents with sudden right-sided weakness and drooping of the left eyelid. Examination shows left eye ptosis, dilated pupil, and right hemiplegia.
Explanation:
Lesion in ventromedial midbrain affecting:
- Oculomotor nerve (III)
- Corticospinal tract
Usually due to posterior cerebral artery infarct
Management:
- Acute ischemic stroke protocol
- Antiplatelet therapy
- Blood pressure and glucose control
- Physiotherapy for hemiplegia
2. Benedikt Syndrome
Case Scenario:
A patient has ipsilateral oculomotor palsy with contralateral tremor and ataxia.
Explanation:
Lesion in tegmentum of midbrain involving:
- Oculomotor nerve
- Red nucleus
- Medial lemniscus
Management:
- Treat stroke or tumor cause
- Antiplatelets or anticoagulation
- Rehabilitation for ataxia
3. Claude Syndrome
Case Scenario:
A patient presents with ipsilateral third nerve palsy and contralateral limb ataxia.
Explanation:
Combination of Weber + Benedikt
- Oculomotor nerve
- Red nucleus
- Corticospinal tract
Management:
- Stroke management
- Neurorehabilitation
4. Parinaud Syndrome
Case Scenario:
Young adult with inability to look upward and light-near dissociation.
Explanation:
Lesion in dorsal midbrain (pineal region)
Often due to pineal tumor or hydrocephalus.
Management:
- Treat raised intracranial pressure
- Neurosurgical tumor management
5. Nothnagel Syndrome
Case Scenario:
Patient has ipsilateral third nerve palsy and cerebellar ataxia.
Explanation:
Lesion of superior cerebellar peduncle + oculomotor nerve
Management:
- Tumor or demyelination treatment
- Supportive therapy
PONTINE SYNDROMES
6. Millard-Gubler Syndrome
Case Scenario:
A patient shows facial paralysis on left side with right-sided hemiplegia.
Explanation:
Lesion in ventral pons
- Facial nerve (VII)
- Corticospinal tract
Management:
- Stroke care
- Facial physiotherapy
7. Foville Syndrome
Case Scenario:
Inability to abduct eye, facial weakness, and contralateral hemiplegia.
Explanation:
Lesion in pontine tegmentum
- Abducens nucleus
- Facial nerve
- Corticospinal tract
Management:
- Antiplatelets
- Eye care for diplopia
8. Raymond Syndrome
Case Scenario:
Ipsilateral lateral rectus palsy with contralateral hemiplegia.
Explanation:
Lesion affects:
- Abducens nerve
- Corticospinal tract
Management:
- Stroke treatment
- Physical rehabilitation
9. Lateral Pontine Syndrome (AICA)
Case Scenario:
Patient presents with facial paralysis, loss of pain and temperature on contralateral body, and vertigo.
Explanation:
AICA infarct affects:
- Facial nerve
- Spinothalamic tract
- Vestibular nuclei
Management:
- Antiplatelets
- Symptomatic vertigo treatment
10. Locked-In Syndrome
Case Scenario:
Patient is conscious but cannot move limbs or speak, only vertical eye movements preserved.
Explanation:
Bilateral lesion of ventral pons
- Corticospinal
- Corticobulbar tracts
Management:
- Supportive ICU care
- Communication aids
- Prevention of complications
MEDULLARY SYNDROMES
11. Lateral Medullary Syndrome (Wallenberg)
Case Scenario:
Patient has dysphagia, hoarseness, ipsilateral facial pain loss, and contralateral body pain loss.
Explanation:
PICA infarct affects:
- Nucleus ambiguus
- Spinothalamic tract
- Inferior cerebellar peduncle
Management:
- Airway protection
- Nasogastric feeding
- Stroke management
12. Medial Medullary Syndrome (Dejerine)
Case Scenario:
Contralateral hemiplegia with loss of proprioception and ipsilateral tongue deviation.
Explanation:
Anterior spinal artery infarct involving:
- Hypoglossal nerve
- Corticospinal tract
- Medial lemniscus
Management:
- Antiplatelets
- Speech therapy
13. Jackson Syndrome
Case Scenario:
Patient presents with ipsilateral hypoglossal paralysis and contralateral hemiplegia.
Explanation:
Lesion affects:
- Hypoglossal nerve
- Corticospinal tract
Management:
- Treat underlying lesion
- Rehabilitation
14. Avellis Syndrome
Case Scenario:
Hoarseness with contralateral loss of pain and temperature.
Explanation:
Lesion affects:
- Nucleus ambiguus
- Spinothalamic tract
Management:
- Swallowing therapy
- Stroke care
15. Babinski-Nageotte Syndrome
Case Scenario:
Features of lateral medullary syndrome plus contralateral hemiplegia.
Explanation:
Extension of lateral medullary lesion into corticospinal tract.
Management:
- Stroke management
- Physiotherapy
MIXED AND FUNCTIONAL BRAINSTEM SYNDROMES
16. Central Pontine Myelinolysis
Case Scenario:
Alcoholic patient develops acute quadriplegia after rapid sodium correction.
Explanation:
Demyelination of central pons due to osmotic injury.
Management:
- Slow correction of sodium
- Supportive care
17. Brainstem Glioma
Case Scenario:
Child presents with cranial nerve palsies and long tract signs.
Explanation:
Diffuse intrinsic pontine glioma compresses nuclei.
Management:
- Radiotherapy
- Steroids
18. Multiple Sclerosis Brainstem Lesion
Case Scenario:
Young female with internuclear ophthalmoplegia and sensory symptoms.
Explanation:
Demyelination of medial longitudinal fasciculus.
Management:
- High-dose steroids
- Disease-modifying therapy
19. Syringobulbia
Case Scenario:
Patient has dissociated sensory loss in face with dysphagia.
Explanation:
Extension of syrinx into brainstem.
Management:
- Neurosurgical decompression
20. Brainstem Encephalitis
Case Scenario:
Fever, altered sensorium, and multiple cranial nerve palsies.
Explanation:
Inflammatory involvement of brainstem nuclei.
Management:
- Antivirals or antibiotics
- ICU monitoring
ADDITIONAL HIGH-YIELD CASE SCENARIOS
21. Inferior Alternating Hemiplegia
22. Superior Alternating Hemiplegia
23. Pontine Hemorrhage
24. Vertebrobasilar Insufficiency
25. Brainstem Abscess
26. Cavernous Hemangioma of Brainstem
27. Progressive Bulbar Palsy
28. Motor Neuron Disease with Brainstem Involvement
29. Trauma-Induced Brainstem Lesion
30. Metabolic Brainstem Dysfunction
(Each presents with characteristic cranial nerve palsies + long tract signs and is managed by treating the underlying cause with supportive neurocritical care.)
Key Exam Tip
> Brainstem syndromes always show “crossed findings” – ipsilateral cranial nerve palsy with contralateral motor or sensory deficit.
FAQ (SEO-Friendly)
Q1. Which artery causes lateral medullary syndrome?
Posterior inferior cerebellar artery (PICA).
Q2. Most common brainstem stroke?
Lateral medullary syndrome.
Q3. Why is locked-in syndrome unique?
Consciousness preserved with complete paralysis.
Q4. Which nerve is involved in medial medullary syndrome?
Hypoglossal nerve.