✅ BODY FLUID COMPARTMENTS (Detailed)
Total body water (TBW) is distributed into different compartments.
1. TOTAL BODY WATER (TBW)
Definition
Total amount of water present in the body.
Normal Values
- Adult Male: ~60% of body weight
- Adult Female: ~50% (more fat tissue)
- Infants: ~75%
Example
A 70 kg man:
[
TBW = 0.6 \times 70 = 42 L
]
So total water = 42 liters
✅ FLUID COMPARTMENTS DIVISION
TBW is divided into:
A. INTRACELLULAR FLUID (ICF)
Definition
Fluid inside all body cells.
Percentage
- 2/3 of TBW
Volume (70 kg male)
[
ICF = 28 L
]
Major ions inside cells
- K⁺ (Potassium)
- Mg²⁺
- Phosphate (PO₄³⁻)
- Proteins
B. EXTRACELLULAR FLUID (ECF)
Definition
Fluid outside cells.
Percentage
- 1/3 of TBW
Volume
[
ECF = 14 L
]
Major ions outside cells
- Na⁺ (Sodium)
- Cl⁻ (Chloride)
- HCO₃⁻
✅ ECF SUBDIVISIONS
1. INTERSTITIAL FLUID
Definition
Fluid between cells (tissue fluid).
Percentage
- 75% of ECF
Volume
[
Interstitial = 10.5 L
]
2. PLASMA (Intravascular fluid)
Definition
Fluid inside blood vessels.
Percentage
- 25% of ECF
Volume
[
Plasma = 3.5 L
]
3. TRANS-CELLULAR FLUID (Small compartment)
Examples
- CSF
- Pleural fluid
- Peritoneal fluid
- Synovial fluid
- Aqueous humor
Normally 1–2 L
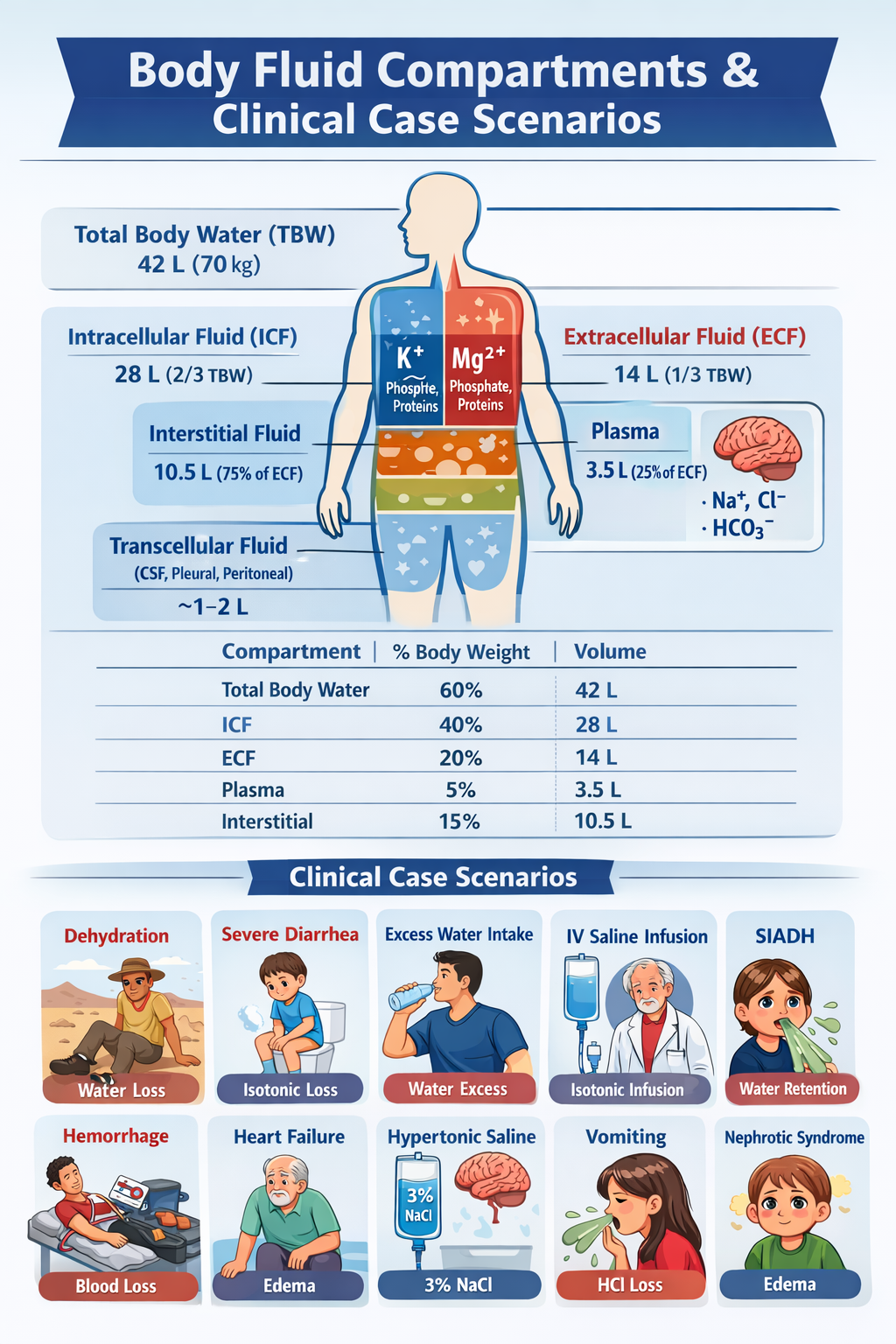
✅ SUMMARY TABLE (70 kg male)
| Compartment | % Body Weight | Volume |
| ---------------- | ------------- | ------ |
| Total Body Water | 60% | 42 L |
| ICF | 40% | 28 L |
| ECF | 20% | 14 L |
| Plasma | 5% | 3.5 L |
| Interstitial | 15% | 10.5 L |
✅ CASE SCENARIOS (VERY IMPORTANT)
Now we apply compartments in clinical physiology.
🔥 CASE 1: Pure Water Loss (Dehydration)
Scenario
A 25-year-old man is lost in desert for 2 days without water.
What happens?
- Water loss > salt loss
Compartment changes
- ECF volume decreases
- Osmolarity increases → water moves from ICF → ECF
- ICF also decreases
Type
Hyperosmotic Volume Contraction
Symptoms
- Thirst
- Dry mouth
- Tachycardia
- Confusion
🔥 CASE 2: Severe Diarrhea
Scenario
A child has watery diarrhea for 3 days.
Fluid lost
- Isotonic fluid from ECF
Compartment changes
- Only ECF decreases
- ICF unchanged
Type
Isosmotic Volume Contraction
Signs
- Hypotension
- Sunken eyes
- Weak pulse
🔥 CASE 3: Excess Water Intake (Psychogenic Polydipsia)
Scenario
A psychiatric patient drinks 10 L water/day.
What happens?
- Osmolarity decreases
Compartment changes
- Water moves into cells
- ICF increases
- ECF increases
Type
Hyposmotic Volume Expansion
Danger
- Cerebral edema → seizures
🔥 CASE 4: IV Normal Saline Infusion
Scenario
A patient receives 2 liters of 0.9% NaCl.
Fluid type
Isotonic
Distribution
- Stays in ECF only
Changes
- ECF increases
- Plasma volume increases
- ICF unchanged
Type
Isosmotic Volume Expansion
🔥 CASE 5: SIADH (Excess ADH)
Scenario
A cancer patient develops SIADH → retains water.
Effect
- Water retention without salt
Changes
- ECF expands
- Water enters ICF → swelling
Type
Hyposmotic Volume Expansion
Symptoms
- Hyponatremia
- Confusion
- Seizures
🔥 CASE 6: Hemorrhage (Blood Loss)
Scenario
A man loses 1.5 L blood in accident.
Fluid lost
Isotonic from plasma
Changes
- Plasma volume ↓↓↓
- Interstitial may shift fluid into plasma
- ICF unchanged initially
Type
Isosmotic Volume Contraction
Signs
- Shock
- Low BP
- Cold clammy skin
🔥 CASE 7: Congestive Heart Failure (CHF)
Scenario
A patient with CHF develops edema.
Cause
- Reduced cardiac output → RAAS activation
- Sodium + water retention
Changes
- ECF expansion
- Plasma leakage → edema
Type
Hypervolemic State
Signs
- Leg swelling
- Pulmonary edema
🔥 CASE 8: Severe Vomiting
Scenario
Patient with pyloric stenosis vomiting for days.
Fluid lost
- HCl-rich fluid → ECF volume loss
Changes
- Metabolic alkalosis
- Hypochloremia
- Volume contraction
🔥 CASE 9: Hypertonic Saline Infusion
Scenario
ICU patient receives 3% NaCl.
Effect
- Osmolarity increases
- Water shifts from ICF → ECF
Changes
- ECF expands greatly
- ICF shrinks
Type
Hyperosmotic Volume Expansion
🔥 CASE 10: Edema in Nephrotic Syndrome
Scenario
Child with nephrotic syndrome has periorbital edema.
Mechanism
- Albumin loss → ↓ plasma oncotic pressure
- Fluid shifts plasma → interstitial
Result
- Plasma volume low
- Interstitial volume high (edema)
✅ KEY EXAM CONCEPTS
Isotonic fluid changes → Only ECF affected
Hypotonic fluid changes → Both ECF + ICF expand
Hypertonic fluid changes → ECF expands, ICF shrinks
✅ QUICK MEMORY FORMULA
- TBW = 60% BW
- ICF = 2/3 TBW
- ECF = 1/3 TBW
- Plasma = 1/4 ECF
- Interstitial = 3/4 ECF